PARKINSON’S DISEASE
Written by Slawomir Gromadzki (“Swavak”), MPH

Autoimmune diseases, including Parkinson’s disease, cause immense suffering and pain. In people who suffer from various autoimmune conditions, the immune system produces antibodies that attack the body’s own tissues. There are over 100 types of autoimmune diseases categorized by the different parts of the body that are affected.
Parkinson’s disease is a progressive autoimmune neurological condition caused by own immune system attacking and destroying dopamine producing cells in the brain. It leads to dopamine deficiency and various symptoms including tremor, slow movements, muscular rigidity, depression, etc.
Parkinson’s particularly affects a region of the basal ganglia called the substantia nigra that utilizes dopamine as its primary neurotransmitter. Neuronal damage and loss in this region is associated with brain cell inflammation and the formation of cross-linked proteins called Lewy bodies in the remaining nerve cells. Lewy bodies block normal cellular activity (>, >).
SYMPTOMS
Parkinson’s disease is a progressive nervous system disorder associated with decreased dopamine levels and corresponding symptoms thataffect movement, starting with small tremors, stiffness or slowing of movement, little or no facial expressions, soft or slurred speech. These symptoms worsen as the condition progresses over time.
POSSIBLE KEY CAUSES
– Vitamin D3 deficiency contributes to all autoimmune diseases! There is a growing amount of research which suggests that a lack of vitamin D could be an important factor in causing autoimmune diseases. Almost every person in England is deficient in vitamin D which is very important for human nervous and immune system.
In his bestselling book “China Study” Prof Colin Campbell wrote that, “Autoimmune diseases in general become more common the greater the distance from the equator. This phenomenon has been known since 1922.” This statement leads us to a simple conclusion that Hashimoto disease may have a lot to do with the vitamin D (“sun vitamin”) deficiency as well as the modern unhealthy lifestyle of North America or Europe. Read more about vitamin D >
– Researchers in Finland have found that people with type II diabetes have a staggering 83% greater risk of developing Parkinson’s!!! (>). In that study, scientists followed a group of over 50,000 men and women over a period of 18 years. During that time, 324 men and 309 women developed Parkinson’s disease. Also a Denmark study has confirmed these findings (>). Increased blood sugar is linked to a harmful process called glycation which creates a massive amount of free radicals (>) leading to a vast oxidative damage in the brain and contributing to Parkinson’s and other neuro-degenerative diseases such as Alzheimer’s. This damage is most commonly associated with blood glucose imbalances in the brain, lack of antioxidants, and toxins such as heavy metals as well as pesticides and herbicides (>, >).
– All body cells (including brain cells) have mitochondria (“engines”) that produce energy for them. Lack of antioxidants such as glutathione, SOD, alpha lipoic acid or CoQ10 allows free radicals and oxidative stress to lead to a dysfunctional state of these extremely important power stations. Studies have proved that individuals with Parkinson’s suffer from an advanced state of mitochondrial dysfunction (>,>,>). People with Parkinson’s disease experience a massive cell death of the dopamine producing cells in their brains. It is now known that this effect is initiated by a mitochondrial dysfunction and a huge decrease in glutathione (GSH) levels!
– British researchers have linked users of pesticide fly killers and herbicide weed killers to be twice as likely to develop Parkinson’s (>, >). Most users spray these very dangerous things in their home without knowing it. These toxic chemicals are also found in non-organic fruits and vegetables.
– Increased homocysteine levels might accelerate dopaminergic cell death in Parkinson disease (PD), through neurotoxic effects.
– Magnesium, Zinc, and Selenium deficiency contribute to Parkinson’s.

– Mercury (from dental fillings, tap water, fish, flu shots, etc.) lead, fluoride, and other toxins.
– Food intolerances: Gluten and A1 Casein Allergy. Dramatic Recovery In Parkinson’s Patient with Gluten Free Diet >
– Exposure to pesticides increases the risk of Parkinson’s disease.
– Hormonal Imbalances: Too much Cortisol (from stress).
– Stress, anxiety and depression. A number of published papers have shown that stress and negative emotions contribute to all autoimmune diseases.

– Consumption of trans fats, margarine and bad oils (high in proinflamatory omega 6) and deficiency of omega 3 healthy fats high in foods such as Flax seed, Chia seed, etc..
– Bad lifestyle, unhealthy diet high in sugar, processed refined foods, nutritional deficiencies, artificial sweeteners, lack of exercise, stimulants, drugs, medication, and in particular excessive stress, depression and pessimism may lead to the oversensitivity of the immune system which changes its nature and starts attacking own body.
– Consumption of meat and dairy products (can trigger autoimmune response and causes hormonal imbalance), refined, junk and processed foods, refined sugar, white flour products, high glucose (high fructose) syrup, stimulants (including coffee, tea, green tea, cola, etc., nutritional deficiencies, white pasta, white rice, processed foods, stress, lack of exercise, etc.
– According to Dr Michael Greger, “Alkylphenols, flame-retardant chemicals, and perfluorochemicals, industrial pollutants found mostly in fish and meat, may be associated with thyroid disruption in young children and adults. Alpha-gal antibodies in meat may result in autoimmune conditions. The artificial food coloring Red No. 3, too much seaweed of any type, and processed meat consumption may be linked to an increase risk of thyroid cancer. Poultry workers often have thyroid disorders.”
– Deficiency of probiotic bacteria in the gut may contribute to PD. The gut and the brain are pretty far apart, but increasingly scientists are connecting the dots and finding that Parkinson’s is truly related to gut bacteria. Read more >
TREATMENT
CONVENTIONAL TREATMENT
L-dopa – a synthetic form of dopamine is the most frequently prescribed medication for Parkinson’s. Although it often produces some short-term symptomatic benefits yet the problem is that it never leads to recovery because it doesn’t addresses the underlying causes of this condition including mitochondrial dysfunction, nutritional deficiencies, high levels of toxins, or oxidative stress in the brain. In addition, L-dopa causes nausea and deficiency of nutrients that are precursors to major neurotransmitters including serotonin (best antidepressant and feel good hormone), L-tryptophan (precursor of serotonin), L-tyrosine, Vitamin B6, or sulphur compounds that are required to produce glutathione (>, >, >, >). These side effects lead to other neurological problems and mood disorders (mostly triggered by reduced serotonin levels). Research gives evidence that L-dopa causes a long-term worsening of the Parkinson’s disease (>).
ALTERNATIVE (NATURAL) TREATMENT
Autoimmune conditions are treated with harmful medication, which have bad side effects. Fortunately it is possible to recover from autoimmune diseases by practicing healthy lifestyle and using natural remedies. The most important element of the treatment is implementing principles from the HEALTH RECOVERY PLAN >
– Find out how to INCREASE DOPAMINE >
– Since it is now known that Parkinson’s is initiated by a mitochondrial dysfunction and a huge decrease in glutathione (GSH) levels you must boost glutathione >
– Increase number of mitochondria in the brain cells and improve mitochondrial function by regular exercise and supplementing most powerful antioxidants such as alpha lipoic acid and CoQ10 >
HERBAL REMEDIES & SUPPLEMENTS
– Research has found that activated charcoal is a very effective in removing pesticides, herbicides and other organic toxins from the body (>)
– Detoxify your body from heavy metals using: Chlorella, Milk Thistle, Turmeric, Cilantro and Charcoal.
– Increased homocysteine levels might accelerate dopaminergic cell death in Parkinson disease (PD), through neurotoxic effects. Higher dietary intakes of folate, vitamin B12, and vitamin B6 (cofactors in homocysteine metabolism) might decrease the risk of PD through decreasing plasma homocysteine. Moreover, vitamin B6 might influence the risk of PD through antioxidant effects unrelated to homocysteine metabolism and through its role in dopamine synthesis. Read more >
– Ginkgo biloba extract may reduce the neurotoxic effects of levodopa in Parkinson’s disease.
– A polysaccharide obtained from Spirulina platensis plays a protective role against the loss of dopaminergic neurons in PD. >
– A study demonstrated that the extract of Ashwaganda may be helpful in protecting the neuronal injury in Parkinson’s disease. > Ashwagandha normalizes catecholamines (compounds that include neurotransmitters) and reduces oxidative damage and physiological abnormalities in a Parkinson’s disease (>).
– Apart from Ashwaganda you can use other herbal remedies and adaptogens such as Rhodiola and Three Tulsi (Holy Basil) tea or capsules.
– Curcumin and naringenin (bitter flavanone in grapefruit, and variety of fruits and herbs) exhibit neuroprotective properties in an animal model of Parkinson’s disease. >
– Boost Glutathione levels which is a most powerful of all antioxidants and strengthens the immune system and is one of the most effective remedies against autoimmune diseases. It boosts body’s ability to modulate and regulate the immune system. It is also important to provide body with ingredients that increase glutathione production in the liver by taking turmeric, milk thistle, NAC (N-acetyl cysteine), bioactive whey protein, Glutamine, Alpha Lipoic Acid, bilberry, vitamin C, asparagus, broccoli, peaches, avocado, spinach, garlic, squash, grapefruit.
– A naturally occurring L-Dopa rich plant extract of Mucuna pruriens was found to be an effective treatment for patients with Parkinson’s disease. Read more >
– Taking selenium supplements and increasing consumption of foods high in selenium (Brazil nuts, sunflower seeds, mushrooms, garlic, onions, etc.).
– Supplement magnesium (800 mg of magnesium citrate a day). Evidence is overwhelming that low levels of magnesium contribute to the heavy metal deposition in the brain that precedes multiple sclerosis, Parkinson’s, and Alzheimer’s. Many of the symptoms of Parkinson’s can be controlled with high magnesium supplementation. In a trial with 30 epileptics 450 mg of magnesium daily doses successfully controlled seizures. Another study found that the lower the magnesium blood levels the more severe was the epilepsy. In most cases magnesium works best in combination with vitamin B6 and zinc.
– Take good quality omega 3 fish oil supplements (Viridian makes an excellent liquid organic omega 3 fish oil with antioxidant to prevent oxidation): 1000-2000 mg a day with meal.
– Vitamin B12 (number one vitamin to prevent and reverse brain nerve damage): 2,000 mcg a day under the tongue (must be sublingual Methylcobalamin!). Many people with neurological and autoimmune diseases have low levels of this most important vitamin. Read a fascinating article on B12 >
– Zinc (helps produce thyroid hormone) – 30 to 50mg a day after breakfast.
– Take good quality probiotic formulas or make raw sauerkraut at home >
– You must take Vitamin D3 because almost all patients suffering from autoimmune diseases patients are deficient in Vitamin D! While using vitamin D3 supplements always remember to take also well absorbed magnesium (such as citrate) as vitamin D supplements are useless without enough magnesium in the body and also lead to magnesium deficiency over time. If you can’t afford higher doses take at least 4,000 IU of vitamin D3 a day with first meal. But since deficiency of this vitamin is so widespread (especially in the UK) it would be better to take 10,000 to 30,000 IU a day with meals with appropriate doses of magnesium. Another requirement for proper absorption of vitamin D is 200 mcg of Vitamin K2 MK-7 (Derived from Natural Natto) a day. Read more about vitamin D > The most important way of obtaining vitamin D is of course through regular sun exposures during summer time between 10am and 2pm. Vitamin D has properties that defend against cell injury caused via free radicals and it affects detoxification pathways which are of importance in disc cell nutritional balance. Vitamin D also affects sensory neurons to modulate pain, influences neuron excitability and acts at the level of substantia gelatinosa and spinal ganglion in the process of sensory perception. Since vitamin D supplements lead to magnesium deficiency, and because according to recent studies almost every in the UK person is now deficient not only in vitamin D but also magnesium, you must take 400 to 800mg of good quality magnesium every day. In addition, if you don’t have enough magnesium in your body (most people don’t) the vitamin D as it needs magnesium for its conversion in your body!
– Alpha lipoic acid: 600-1200 mg per day in 2 doses. Alpha lipoic acid has proven its ability to prevent oxidative stress caused by radicals and other factors in nerve tissue. It helps to maintain high glutathione levels which are found to be depleted in individuals diagnosed with Parkinson’s disease. Current research also reveals protective effects of alpha lipoic acid in neuropathy, excitotoxic amino acid brain injury, mitochondrial dysfunction, and other causes of damage to neural or brain tissue.
– In Parkinson’s disease higher doses of CoQ10 give excellent results (100 – 300mg of Ubiquinone form a day as there is no difference with regards to absorption between Ubiquinone and Ubiquinol if the first one is oil based and not in the form of dry powder, and if it is taken with meal).
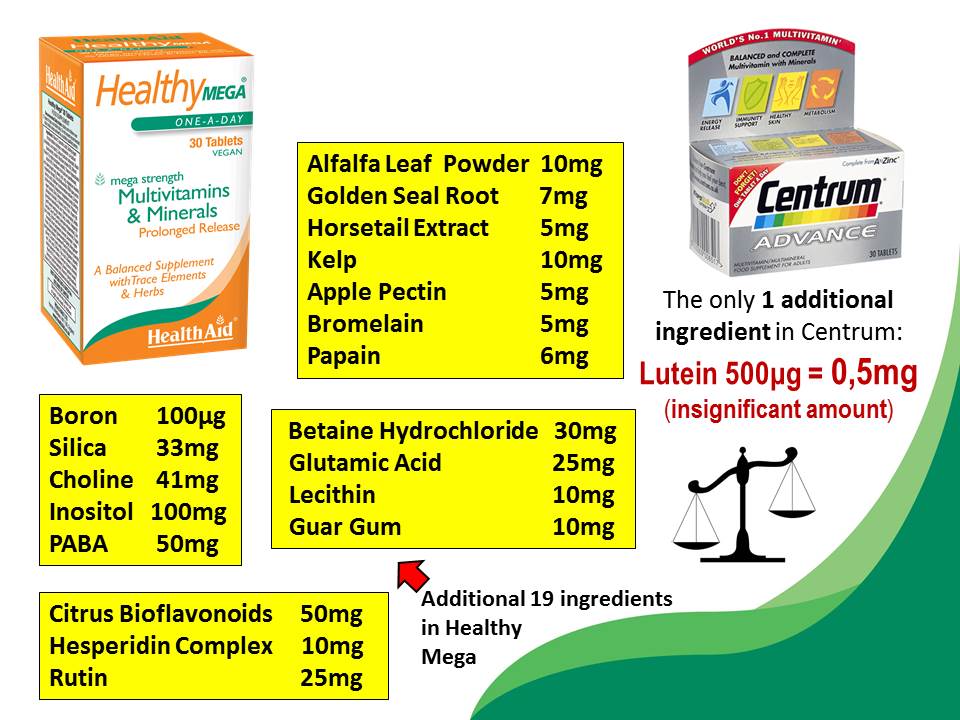
– Good quality multivitamin-mineral formula (high in B vitamins): 1 tablet after breakfast. Please do not buy cheap formulas as their potency is very low and they contain only short list of inorganic ingredients. It must be a good quality formula such as Healthy Mega (HealthAid), VM75 (Solgar) or Special Two (NOW Foods) which are an excellent multi-vitamin and mineral formulas fortified with alfalfa powder, rutin, citrus bioflavonoids, bromelain, herbs, digestive enzymes and many other super nutrients. If your diet is very healthy and you stay away from refined foods, sugar and stimulants then take only 1/2 tablet after breakfast.

– Since Vitamin B complex (B1, B2, B3, B6, B12, Folate) play very important role in dealing with neurological problems I recommend getting B complex in a good quality multivitamin-mineral formula which is high in B vitamins.

– CoQ10 – has been found to improve symptoms for some Parkinson’s patients, and may well be a candidate for adjunctive treatment according to a clinical research. Read more >
– The Rick Simpson Cannabis Oil seems to be the most effective remedy in treating PD. Despite the controversy surrounding medical marijuana use, research has demonstrated that a component of cannabis known as cannabidiol (CBD), and which is free fro psychoactive properties associated with tetrahydrocannabinol (THC), may have a wide range of therapeutic applications, including treating PD. Read more >
Watch VIDEO > demonstrating amazing therapeutic effect of cannabis oil on Prkinson’s disease
According to Dr Joseph Mercola, “In his medical practice, Dr. Frankel treats a wide variety of patients with medical cannabis, which has become his specialty. Despite the many claims of cannabis performing miracles, he’s reluctant to think of it as a cure for anything. Occasionally, however, patients will experience very dramatic results. For example, he has seen tumours virtually disappear in some patients using no other therapy except taking 40 to 60 milligrams of cannabinoids a day. The most common thing he sees in cancer patients, however, are tumours shrinking, or a metastasis disappearing. Sometimes tumours will shrink or vanish, only to re-emerge in other areas, months later, and then shrink or vanish again… Other common ailments being treated with cannabis include: Parkinson’s disease, Multiple sclerosis, Degenerative neurological disorders such as dystonia, Mood disorders, and Pain disorders.”
NUTRITIONAL AND LIFESTYLE RECOMMENDATIONS
Autoimmune diseases can be reversed by practicing the following guidelines:
– Avoid gluten. According to the Greenmedinfo, “A remarkable new case report describing the dramatic recovery of a 75-year-old Parkinson’s disease patient after following a 3-month long gluten free diet reveals the need to explore whether there is an increased prevalence of silent or symptomatic celiac disease or non-celiac gluten sensitivity both in those afflicted with Parkinson’s disease and the related multi-factorial neurodegenerative condition known as Parkinsonism.” Read more >
– If possible, avoid all animal foods including cheese, meat products, all dairy, stimulants (caffeine, alcohol, cigarettes, etc.).
– The key to reverse Parkinson’s is an anti-inflammatory diet and lifestyle. This includes lots of clean water and phytonutrient rich raw and lightly cooked vegetables, good fats such as raw coconut oil, avocados, olive oil, and nuts/seeds. Avoid hydrogenated fats, trans fats (margarines, doughnuts, cakes, etc.) and proinflamatory omega 6 fatty acids (soy oil, corn oil, sunflower oil, etc.).
– Strictly plant based unrefined diet such as Hallelujah diet gives best results but if you can’t give up on meat and dairy make sure you consume better quality foods from grass-fed animals or farm free-range chicken.
– Go on vegan unrefined diet as it gives best results. Eat especially with lots of raw vegetables salads and raw vegetable juices.
– Proper stress control and positive thinking – extremely important!
– Eliminate all junk food, processed food, artificial sweeteners, trans fats, and anything with bad preservatives and chemical.
– Eating whole, unprocessed foods, and choosing as many organics as possible.
– Getting adequate sun exposure if possible (20 minutes a day during summer time between 10 am and 2 pm) to maintain vitamin D levels.
– Avoid all dairy products as heated dairy protein (especially A1 casein) often irritates the immune system stimulating it to produce antibodies against different internal organs. The most common allergies and food intolerances today are from wheat and dairy products because of the hybridized proteins of gluten and a1 casein. These proteins can cause Leaky Gut Syndrome which leads to inflammation.
– Use glass bottles as Bisphenol A (BPA) which is found in plastic bottles and cans (they are lined up with plastic) disrupt endocrine system.
– Avoiding chlorine, fluoride (toothpastes with fluoride, etc.), and bromine as they also contribute to autoimmune diseases.
– Increase consumption of omega 3 fatty acids in the form of ground flax seeds, chia seeds. Omega 3s are the building blocks for hormones that control immune function and cell growth.
– Remove any dental fillings containing mercury.
– Increasing intake of healthy fats such as raw coconut oil, coconut milk, avocado, chia seeds (soaked for at least 30 minutes or overnight), ground flaxseed, and hemp seeds as they will balance hormones. Coconut oil is one of the best foods for thyroid. Coconut oil is a saturated fat comprising medium chain triglycerides (MCTs), which are known to increase metabolism and promote weight loss. Coconut oil is very stable (shelf life of three to five years at room temperature), so body is much less burdened with oxidative stress than it is from many other vegetable oils.
– Increase consumption of vitamin A in the form of beta-carotene found in carrots, apricots, green leafy vegetables, etc.
– Eliminate stimulants (anything with caffeine or other similar harmful alkaloids: coffee, tea, green tea, mate, yerba mate, cola, chocolate, etc.).
– Exercise at least 30–60 minutes per day.
– Get enough sleep.
– Practice deep breathing.
– Address adrenal fatigue. A prolonged stress response can lead to adrenal exhaustion (also known as adrenal fatigue). Find out more about ADRENAL FATIGUE >
– Treat unresolved emotional issues as a source of stress. Autoimmune diseases reflect emotions and mental attitude. When people with autoimmune diseases make progress in treating unresolved emotional issues, their symptoms subside. Stress, anxiety or depression are often key culprits. It is important to identify the stressors and learn use ways such as prayer that can help to control stress and negative emotions.
– Read about the DEADLY CONSEQUENCES OF UNFORGIVENESS >
– Drink and use for cooking only distilled or at least filtered water. Not all water filters remove fluoride, so make sure the one you have does or use only distilled water (buy a water distiller). Taking chlorella and turmeric help to get rid of fluoride and heavy metals such as mercury.
Autoimmune Disease Success Stories >
Researchers claim that neuron cell death in Parkinson’s disease may be caused by overactive immune system
June 27, 2016, University of Montreal
“Two genes associated with Parkinson’s disease are key regulators of the immune system, providing direct evidence linking Parkinson’s to autoimmune disease, a new study indicates.”
“A team of scientists from the University of Montreal and the Montreal Neurological Institute and Hospital have discovered that two genes associated with Parkinson’s disease (PD) are key regulators of the immune system, providing direct evidence linking Parkinson’s to autoimmune disease.”
Using both cellular and mouse models, the team has shown that proteins produced by the two genes, known as PINK1 and Parkin, are required to prevent cells from being detected and attacked by the immune system.
When PINK1 and Parkin are dysfunctional, as is the case in a subset of Parkinson’s patients, cells display small parts of proteins at their surface, known as antigens, derived from mitochondria. The presence of these antigens at the cell surface causes the activation of immune cells called lymphocyte T cells. These T cells, which can enter the brain, have the ability to destroy any cell displaying the mitochondrial antigens on their surface.
Parkinson’s is caused by the death of dopamine-producing neurons in the brain. An overactive immune system due to dysfunctional PINK1 and Parkin genes could explain why dopaminergic neurons die in Parkinson’s patients. This indicates that Parkinson’s may be one of many autoimmune diseases, including multiple sclerosis, Type 1 diabetes, rheumatoid arthritis, and lupus. An autoimmune disease is one in which the body’s own immune system attacks healthy cells.
Researchers suspected that mitochondria, organelles within cells that are responsible for the production of energy and other metabolites, play a role in Parkinson’s. It was widely believed that mitochondria become damaged in Parkinson’s patients, creating a toxic build-up of broken mitochondria that eventually leads to neuron cell death. However, it has been difficult to provide evidence that this is effectively happening in animal models.
The new findings of the Desjardins/McBride teams linking PD to autoimmune mechanisms, published in the journal Cell on June 23, have been validated in a mouse model of Parkinson’s disease where PINK1 or Parkin are absent.
“Clinicians have shown that the immune system is activated in the brain of PD patients,” says Dr. Diana Matheoud, a postdoctoral fellow from the University of Montreal and the article’s first author. “Our study explains how an attack by the immune system may be responsible for the destruction of dopaminergic neurons during the disease. We are currently testing whether autoimmune mechanisms lead to the loss of dopaminergic neurons in mice, and developing systems to extend our study to human neurons.”
“Antigen presentation was not believed to play a direct role in Parkinson’s disease,” says McBride. “While most laboratories are following the trail of the ‘toxic mitochondria’ model, our path led us to observe Parkinson’s disease from a different point of view. Our approach, centered on the immune system, led us down a different road where we were able to observe that autoimmunity is likely to play an important role in the progression of the disease.”
Now that a link has been established between two key genes involved in the pathology of Parkinson’s disease and autoimmune mechanisms, the next step is to develop drugs that can limit the presentation of mitochondrial antigens. Remarkably, the mechanism by which mitochondrial antigens are presented involves a process of vesicle formation, originally described by the McBride group, offering molecular targets for the development of new drugs in an effort to block this process.
The researchers’ findings may also lead to better treatments for other diseases. “We think that our study is paradigm shifting because we have identified a new biological pathway linking mitochondria to immune mechanisms in Parkinson’s disease. This opens the possibility to use therapies based on modulation of the immune system, something already done for the treatment of other diseases,” says Desjardins. “Interestingly, the role played by PINK1 and Parkin in limiting the presentation of mitochondrial antigens may not only regulate a process that impact Parkinson’s disease, but may also affect other autoimmune diseases like diabetes and lupus, and primary biliary cirrhosis, where a link to mitochondrial antigen presentation has been observed.”
“This paper suggests an entirely novel mechanism by which these recessive, inherited mutations may lead to neurodegeneration,” says Jon Stoessl, Professor and Head of Neurology at the University of British Columbia & Vancouver Coastal Health, and former Director of the Pacific Parkinson’s Research Centre. “There has been much interest in the potential role of inflammation in PD. Previous studies on Parkin and PINK1 have focused on disruption of mitochondrial housekeeping functions. While the current findings may clearly be related, they suggest an entirely novel approach to the development of targeted therapies. It should be remembered that these are rare causes of Parkinson’s disease and the relevance to dominantly inherited and sporadic forms of disease remains to be determined.”
Story Source: The above post is reprinted from materials provided by University of Montreal. Note: Materials may be edited for content and length.
References
Diana Matheoud, Ayumu Sugiura, Angélique Bellemare-Pelletier, Annie Laplante, Christiane Rondeau, Magali Chemali, Ali Fazel, John J. Bergeron, Louis-Eric Trudeau, Yan Burelle, Etienne Gagnon, Heidi M. McBride, Michel Desjardins. Parkinson’s Disease-Related Proteins PINK1 and Parkin Repress Mitochondrial Antigen Presentation. Cell, 2016; DOI: 10.1016/j.cell.2016.05.039
Contrary to decades of research suggesting Parkinson’s disease behaves one way, a new study from Columbia University proposes an alternate disease profile that moves the affliction away from being entirely a neurological disorder and toward that of an autoimmune disease.
The idea, while controversial, suggests that when neurons die, they’re doing it specifically because the antigens (or bacteria) on the surface of the neurons are being displayed. This allows the body’s T cells, which mediate immunity, to attack the antigen, thereby mistakenly killing the neuron. Up until this research, neurons weren’t thought to display any antigens, meaning the immune system wouldn’t respond. But new data presents a contrary view to this deep-seated belief.
For a long time, scientists believed T cell attacks were no match for the brain’s neurons. “That idea made sense because, except in rare circumstances, our brains cannot make new neurons to replenish ones killed by the immune system,” explained Dr. David Sulzer, the study’s senior author and Columbia professor of neurobiology, in a statement. It wouldn’t make sense, in other words, for the brain to allow its own cells to die, essentially by surrendering. “But, unexpectedly, we found that some types of neurons can display antigens.”
Most cells, when they’re infected by a virus or invading bacteria, reveal pieces of it on their surface. Parkinson’s is an interesting case because scientists still don’t understand the cause of neuronal death — the why. What the present study offers is insight into thehow. Sulzer and his team believe the body’s immune system mistakes neurons as foreign invaders, similar to other cells in the case of type I diabetes, celiac disease, andmultiple sclerosis, before killing the cells in hopes of eradicating the “virus.”
The problem, of course, is that there is no virus. To understand why the immune system may behave like this, the research team used healthy postmortem brain tissue to analyze the nature of the T cell attacks. They specifically looked at a set of cell surface molecules called major histocompatibility complex (MHC) molecules, which are present when the antigen is displayed. They found, to their surprise, MHC proteins in two types of neurons. Both of these neurons degenerate during Parkinson’s disease.
“Right now, we’ve showed that certain neurons display antigens and that T cells can recognize these antigens and kill neurons,” Dr. Sulzer said, “but we still need to determine whether this is actually happening in people. We need to show that there are certain T cells in Parkinson’s patients that can attack their neurons.”
AN ATTEMPT TO SOLVE THE MYSTERY OF AN AUTOIMMUNE RESPONSE
Autoimmune diseases are becoming extremely common nowadays, especially among women. Researchers have proved that all autoimmune disorders basically reflect the same strange phenomenon: The irritated and weakened by different factors (including unhealthy diet, dairy, gluten, toxins, stress, or vitamin D deficiency) immune system, mistakes healthy tissue or organs as foreign and begins to attack them. The only difference between numerous autoimmune diseases is the type of organ or tissue which is attacked. In case of vitiligo, eczema or psoriasis it is skin; in Parkinson’s disease it is dopamine producing brain cells; in lupus it can be different parts of the body including joints, skin, liver, etc. When leukocytes attack pancreas they cause type I diabetes. With ulcerative colitis and Crohn’s disease, it is the colon; and with multiple sclerosis, it is the nerve cells of the brain and spinal cord. In case of Hashimoto’s hypothyroidism and Graves’ hyperthyroidism, the thyroid is the target of the immune system.
It is very interesting that Hashimoto’s disease (the most common cause of underactive thyroid) as well as Grave’s disease (the most common cause of overactive thyroid) are both an autoimmune conditions. However, there is an important difference between these two diseases with regards to the role and influence of the immune system: In Hashimoto’s leukocytes, instead of protecting the gland, strangely treat thyroid cells as if they were some dangerous invaders and destroy thyroid cells making them unable to produce enough hormones. In Grave’s disease, on the other hand, white blood cells go into another extreme, and although there is no physiological need to do this, they stimulate thyroid to make way too much of its hormones.
It means that in both cases the immune system gets “crazy” and instead of protecting thyroid cells it behaves in a very strange way and either decides to kill thyroid gland or cause another harm by forcing overproduction of thyroid hormones!
Unfortunately, it is almost impossible to find a medical website or a scientist that would at least attempt to explain this extremely weird behaviour of human immune system. They are unable to do it probably because scientists look for a very complex scientific answers while the solution may be surprisingly simple and logical. Apart from that, for them the immune system is just a bunch of unintelligent cells that came into existence as a result of evolution and only mechanically perform their physiological functions.
Fortunately, back in Poland I was very lucky to have a privilege of translating a series of health lectures by American physician Dr. Sang Lee who developed a very interesting explanation of this phenomenon. So let me try to share with you a few thoughts I still remember from his fascinating and unique health seminars.

When we carefully study the physiology of our immune system we quickly get an impression that somehow our immune system behaves in an incredibly intelligent way. It is also clear that the immune system is very closely connected to the brain and nervous system and that white blood cells respond to different physiological and even psychological needs. One scientist trying to express this idea even suggested that leukocytes behave like “pieces of brain scattered all over the body”.
There is no doubt brain is the most important part of human body. Brain in our organism is like a “king” or a “boss” and because of that, no cell, including the immune system cells ever question any information, signals or anything coming from the brain. That is why the placebo or nocebo effect (a positive or negative attitude of the brain) can impose such a powerful effect on body’s physiology and health.
Knowing this we can draw some very important conclusions which will help us to understand how mental attitudes and emotions can influence the immune system cells to either destroy thyroid or stimulate it to make more hormones.
We know that great majority of both hypothyroidism and hyperthyroidism are caused by abnormal and harmful response (behaviour) of the immune system. The autoimmune form of hypothyroidism is called Hashimoto’s disease and in case of hyperthyroidism it is Graves disease.
Another fact we need to take into consideration is that autoimmune diseases (including both thyroid autoimmune conditions) are much more prevalent among women than man, even if their diet and lifestyle are similar. Now, that doesn’t mean bad diet, and lack of exercise do not contribute to the development of autoimmune diseases, but that there is another cause which should be regarded as even more significant.
The simple conclusion, therefore, is that it is anxiety, depression, worrying and negative mental attitudes that must greatly contribute to the development of autoimmune diseases, simply because poor mental health is also much more common among women than men.
Taking into consideration all those facts Dr Lee suggested that when a woman suffers from chronic anxiety or depression, when she has negative attitude toward life, keeps on thinking about death or suicide, or if she is overwhelmed by any other negative thoughts and emotions, her intelligent and closely connected to the brain immune system gets a clear impression that the “boss” (which is the brain) doesn’t want to live. Therefore, like obedient soldiers the white blood cells feel obliged to fulfil the desire of the “boss”, so they turn against its own body and begin to attack different organs. In case of Hashimoto’s disease it is thyroid.
The whole situation is made even more dangerous when a depressed woman does not exercise, and since only dead body does not move, the leukocytes draw a conclusion that she is already dead so why they should protect the dead body? If she is dead it is more reasonable rather to attack the body and accelerate the decaying process!
But, someone may argue that, if pessimism, depression, anxiety, and suicidal thoughts contribute to the development of autoimmune diseases, how to explain that sometimes babies or small children are diagnosed with autoimmune diseases such as lupus, eczema, or type 1 diabetes? They couldn’t trigger these conditions through their pessimism.
The answer is obvious, they either inherited overreacting immune system or their immune system was negatively influenced by mother’s nervous system (depression, anxiety, suicidal thoughts, etc.) when they were in their mother’s womb. There are many women who during pregnancy were depressed or even attempted to commit suicide and gave birth to children who sooner or later were diagnosed with autoimmune diseases. In addition babies are very often deficient in Vitamin D ad are fed with cow’s milk and it is scientifically proved that both factors also contribute to the development of autoimmune diseases in children.
There are also some nutritional ways to trigger an autoimmune reaction. We already know that heated animal protein, especially the one found in cow’s milk and dairy, is often treated by human immune system as a foreign invader. Because of that leukocytes send antibodies against those heated proteins which get into human body with milk and dairy products. The problem however is that in our bodies there are certain proteins which look exactly like those heated milk proteins so the weakened immune system often mistakenly and simultaneously attack also those body’s own proteins, causing different autoimmune problems.
Apart from pessimism and sedentary lifestyle there are still other “death signals” that may “inspire” the immune system to attack own body. For instance, using stimulants such as alcohol, smoking, illegal drugs, coffee, tea, cola, sugar, etc. could be discerned by the immune system as the “death wish” (“death signals”) of the brain and thus “inspire” the immune system with the idea that the “boss” wishes to die (due to the suicidal lifestyle and diet). The immune system may get this impression because stimulants are harmful and toxic chemicals which slowly contribute to the death of the body.
Also regular consumption of meat products may trigger similar reaction because meat comes from dead animals.
In addition, any heated (cocked, boiled, fried, grilled) animal protein always triggers immune reaction causing leukocytes to start mobilising and thus leading to increased number of leukocytes in the blood. This phenomenon is called leucocytosis and has bad influence on the immune system. As a result of frequent consumption of heated animal proteins (cooked dairy, meat, poultry, fish, or eggs) the immune system is frequently alarmed, has to overwork and may change its nature. Eventually it often turns against its own body causing numerous autoimmune diseases, including thyroid problems.
In case of the Graves hyperthyroidism, however, the behaviour of the immune system seems to be very opposite than in Hashimoto’s thyroiditis or other autoimmune conditions because in Graves hyperthyroidism instead of attacking and destroying the tissue leukocytes just stimulate thyroid to make even more hormones! Now, why on earth in this case the immune system changed its tactics and instead of killing thyroid gland it just decides to “help” it to work very hard?
Well, also in this case Dr Lee got a very interesting explanation. He suggests that if a woman lives a very stressful lifestyle, always tries to do her best in performing her duties at home and work, often in a hurry, dealing with many different things at the same time, if she doesn’t rest and sleep long enough at night, gets often nervous or irritated, drinks coffee or uses other stimulants to increase her energy so that she could be more efficient, then guess what the “intelligent” immune system, which responds to the physiological and psychological needs, do? The immune system says, “Ok, the boss is very restless, wants be more energetic and efficient in performing different duties, let us then go to thyroid and stimulate it to make more hormones, and in this way we will fulfil the wish of the boss.” When over a decade ago I heard this idea for the fists time I said, “Wow! It is so fascinating how our immune system works and how it can be influenced by mental attitudes!”
Well, if this idea is true, and to be honest I personally like it very much, then the best way to prevent and treat autoimmune diseases (including Hashimoto’s hypothyroidism and Graves hyperthyroidism) is by stress control, positive thinking, laughter, frequent smiling, taking care of others, helping people in need, going for a walk and enjoying life and the beauty of the nature. It can be done by avoiding “death signals” (stimulants, meat products and other heated dead foods, etc.). In this way you will show the immune system that you want to live and actually enjoy life. As a result those smart and intelligent invisible tiny soldiers (the white blood cells) will never attack your own body (or will stop doing that) but will protect and fight for you like Kamikazes.
Unfortunately, from my long experience I know that for many of us it is very difficult and often even impossible to become a positive thinking person because those negative emotions and fears seem to be part of our nature. Sometimes we even feel like slaves of pessimism.
And that sad truth is the very reason I included on my website a very special, unique and even most important section called “EMPOWRNMENT”. So please read it carefully and then study the even more significant article titled the “GOSPEL OF FREEDOM“, as it reveals the secret of finding the only source of true inward “peace” which according to Apostle Paul “surpasses all knowledge” and which can “guard (protect) our hearts and minds (emotions)”.
Combined with true strong faith this message will lead you to freedom from negative emotions such as anxiety or existential fears (one of the key source of deadly free radicals). It will empower you with moral strength necessary to overcome long-cultivated bad habits or addictions, often impossible to defeat on our own. This unique and most wonderful good news of the gospel will also give you a powerful motivation to not only practice but also enjoy the new and very healthy way of life.
SOURCES
Hafström I, Ringertz B, Spångberg A, et al. A vegan diet free of gluten improves the signs and symptoms of rheumatoid arthritis: the effects on arthritis correlate with a reduction in antibodies to food antigens. Rheumatology (Oxford) 2001, 40:1175-1179.
Proudman SM, James MJ, Spargo LD, et al. Fish oil in recent onset rheumatoid arthritis: a randomised, double-blind controlled trial within algorithm-based drug use. Ann Rheum Dis 2013.
Tursi A, Brandimarte G, Papa A, et al. Treatment of relapsing mild-to-moderate ulcerative colitis with the probiotic VSL#3 as adjunctive to a standard pharmaceutical treatment: a double-blind, randomized, placebo-controlled study. Am J Gastroenterol 2010, 105:2218-2227.
Hu G, Jousilahti P, Bidel S, Antikainen R, Tuomilehto J. Type 2 diabetes and the risk of Parkinson’s disease. Diabetes Care. 2007 Apr;30(4):842-7. PMID: 17251276
Schernhammer E, Hansen J, Rugbjerg K, Wermuth L, Ritz B. Diabetes and the risk of developing Parkinson’s disease in Denmark. Diabetes Care. 2011 May;34(5):1102-8. PMID: 21411503
Goldin A, Beckman JA, Schmidt AM, Creager MA. Advanced glycation end products: sparking the development of diabetic vascular injury. Circulation. 2006 Aug 8;114(6):597-605. PMID: 16894049
Zupancic M, Mahajan A, Handa K. Dementia With Lewy Bodies: Diagnosis and Management for Primary Care Providers. The Primary Care Companion to CNS Disorders. 2011;13(5)
Hwang O. Role of Oxidative Stress in Parkinson’s Disease. Experimental Neurobiology. 2013;22(1):11-17
Jenner P. Oxidative stress in Parkinson’s disease. Ann Neurol. 2003;53 Suppl 3:S26-36; discussion S36-8. PMID: 12666096
Parkinson’s disease and pesticide exposures. Dick FD. Br Med Bull. 2006;79-80:219-31.PMID: 17242039
Pesticides and Parkinson’s disease – a critical review Link Here
Winklhofer KF, Haass C. Mitochondrial dysfunction in Parkinson’s disease. Biochim Biophys Acta. 2010 Jan;1802(1):29-44. PMID: 19733240
Merad-Boudia M, Nicole A, Santiard-Baron D, Saillé C, Ceballos-Picot I. Mitochondrial impairment as an early event in the process of apoptosis induced by glutathione depletion in neuronal cells: relevance to Parkinson’s disease. Biochem Pharmacol. 1998 Sep 1;56(5):645-55. PMID: 9783733
Mytilineou C, Kramer BC, Yabut JA. Glutathione depletion and oxidative stress. Parkinsonism Relat Disord. 2002 Sep;8(6):385-7. PMID: 12217624
Harvey CJ, Thimmulappa RK, Singh A, et al. Nrf2-regulated glutathione recycling independent of biosynthesis is critical for cell survival during oxidative stress. Free radical biology & medicine. 2009;46(4):443-453.
Cuadrado A, Moreno-Murciano P, Pedraza-Chaverri J. The transcription factor Nrf2 as a new therapeutic target in Parkinson’s disease. Expert Opin Ther Targets. 2009 Mar;13(3):319-29. PMID: 19236154
Dyall SC. Long-chain omega-3 fatty acids and the brain: a review of the independent and shared effects of EPA, DPA and DHA. Front Aging Neurosci. 2015 Apr 21;7:52. PMID: 25954194
Cardoso HD, dos Santos Junior EF, de Santana DF, Gonçalves-Pimentel C, Angelim MK, Isaac AR, Lagranha CJ, Guedes RC, Beltrão EI, Morya E, Rodrigues MC, Andrade-da-Costa BL. Omega-3 deficiency and neurodegeneration in the substantia nigra: involvement of increased nitric oxide production and reduced BDNF expression. Biochim Biophys Acta. 2014 Jun;1840(6):1902-12. PMID: 24361617
Burbulla LF, Krebiehl G, Krüger R. Balance is the challenge–the impact of mitochondrial dynamics in Parkinson’s disease. Eur J Clin Invest. 2010 Nov;40(11):1048-60. PMID: 20735469
Knekt P, Kilkkinen A, Rissanen H, Marniemi J, Sääksjärvi K, Heliövaara M. Serum vitamin D and the risk of Parkinson’s disease. Archives of neurology. 2010;67(7):808-811.
Murakami K, Miyake Y, Sasaki S, Tanaka K, Fukushima W, Kiyohara C, Tsuboi Y, Yamada T, Oeda T, Miki T, Kawamura N, Sakae N, Fukuyama H, Hirota Y, Nagai M; Fukuoka Kinki Parkinson’s Disease Study Group. Dietary intake of folate, vitamin B6, vitamin B12 and riboflavin and risk of Parkinson’s disease: a case-control study in Japan. Br J Nutr. 2010 Sep;104(5):757-64. PMID: 20338075
Kerksick C, Willoughby D. The Antioxidant Role of Glutathione and N-Acetyl-Cysteine Supplements and Exercise-Induced Oxidative Stress. Journal of the International Society of Sports Nutrition. 2005;2(2):38-44.
Wu G, Fang YZ, Yang S, Lupton JR, Turner ND. Glutathione metabolism and its implications for health. J Nutr. 2004 Mar;134(3):489-92. PMID: 14988435
Foo KY, Hameed BH. Detoxification of pesticide waste via activated carbon adsorption process. J Hazard Mater. 2010 Mar 15;175(1-3):1-11. PMID: 19879688
García NH, Berndt TJ, Tyce GM, Knox FG. Chronic oral L-DOPA increases dopamine and decreases serotonin excretions. Am J Physiol. 1999 Nov;277(5 Pt 2):R1476-80. PMID: 10564221
Hinz M, Stein A, Cole T. The Parkinson’s disease death rate: carbidopa and vitamin B6. Clinical Pharmacology : Advances and Applications. 2014;6:161-169.
Borah A, Mohanakumar KP. Long-term L-DOPA treatment causes indiscriminate increase in dopamine levels at the cost of serotonin synthesis in discrete brain regions of rats. Cell Mol Neurobiol. 2007 Dec;27(8):985-96. PMID: 17934805
Effect of chronically administered L-Dopa on Dopa/5HTP decarboxylase and tyrosine and tryptophan hydroxylases in cat brain Link Here
Sabens EA, Distler AM, Mieyal JJ. Levodopa deactivates enzymes that regulate thiol-disulfide homeostasis and promotes neuronal cell death: implications for therapy of Parkinson’s disease. Biochemistry. 2010 Mar 30;49(12):2715-24. PMID: 20141169
Any information or product suggested on this website is not intended to diagnose, treat, cure or prevent any medical condition. Never disregard medical advice or delay in seeking it because of something you have read on this website. Consult your primary healthcare physician before using any supplements or making any changes to your regime.
© 2016 Slawomir Gromadzki – All Rights Reserved
