OSTEOPOROSIS & OSTEOPENIA
Written by Slawomir Gromadzki, MPH
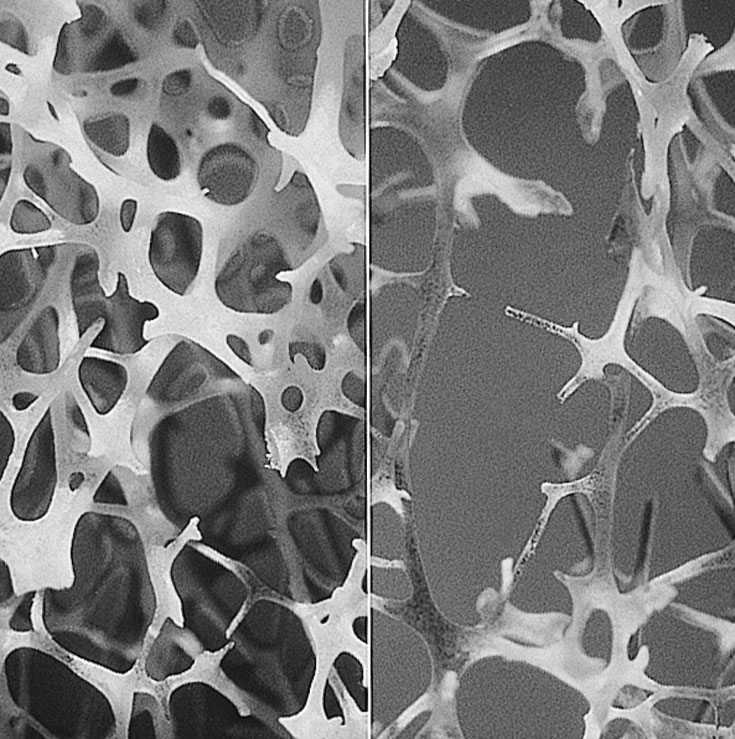
The difference between osteopenia and osteoporosis is that in osteopenia the bone loss is not as severe as in osteoporosis. In this article i address osteoporosis but causes and treatment in both cases are the same.
Osteoporosis is a condition in which the bones become weak and brittle because of the gradual loss of tissue. It is estimated that about 20 million people (mostly postmenopausal women) in the United States alone suffer from osteoporosis. About 50% of those with this condition experience bone fractures. Men are rarely affected due to a greater life-long bone density.
CAUSES
– Osteoporosis is usually caused by hormonal imbalance (low estrogen) and deficiency of vitamin D, vitamin K2, silica, boron, zinc, and magnesium.
– Dairy Products: Because dairy products are high in protein, salt, fat and phosphates, they may actually interfere with the retention of calcium stores and cause more calcium to be lost than saved when they are used in the large amounts usually promoted by the dairy industry. High levels of protein make an acid condition in the blood, tax the organs which must eliminate the excess, and trigger loss of calcium from the bones. The kidneys have to excrete the excess and the wastes left over from metabolism, increasing the risks of developing kidney disease. The calcium excess from so much dairy products may form kidney stones. This process of calcium loss due to dairy consumption is not reserved for those over 35 who have reached peak bone mass and are experiencing age-related bone loss. Even younger people who consume a great deal of dairy have been found to have thinning bones. As dairy consumption in a population goes up, so does osteoporosis. Note the chart below on hip fractures.
– Other causes may include refined diet; lack of exercise; smoking; alcohol; coffee; prescription drugs (especially cortisone, prednisone and their relatives); over-the-counter pain killers; oral contraceptives; lack of sunlight; aluminium or phosphate baking powders; anorexia nervosa; diabetes, rheumatoid arthritis and other bone diseases; sedentary lifestyle or periods of enforced bed-rest;
– Several drugs contribute to osteoporosis: Corticosteroids (cortisone, prednisone and all related steroids), antibiotics especially tetracycline and its derivatives, thyroid hormone supplements such as thyroxin, isoniazid for tuberculosis, tranquilizers and psychotropic drugs such as anti-depressants. Long use of aluminium antacids such as Amphogel, Mylanta, Maalox, Aludrox, Gelusil.
– Free, Inspired, Life-Transforming Book!
– Can Christ Return in 2027
– Aluminium deodorants, aluminium cookware and cans used in canned foods and sodas, and excessive athletic or dance training.
– Nutritional deficiencies: As more studies are being conducted, there is continued evidence that it is the proper intake and combined use of many foods containing different vitamins and minerals that protect one from osteoporosis, not just calcium intake. Vitamins A, C, and D, plus the B vitamins and K, all combine in the growth, repair and maintenance functions in the body. Magnesium, Manganese, Folic Acid, Boron, Strontium, Calcium, Silicon, Zinc, Copper, and Iron all help keep the body in a positive state of balance. Taking heavy supplements, especially of vitamins A and D, can damage the delicate balance in the body, burdening the organs.
– Vitamin D deficiency. Vitamin D enables the body to absorb calcium, but too much synthetic vitamin D can cause heart problems. Low blood levels of vitamin C have been found in people with hip fractures, even when hipbone calcium quantities were the same as those people without fractures. Vitamin C promotes connective tissue in bone. It is on this framework of tissue that bone-hardening calcium is laid. Without adequate supplies of vitamin C, bones cannot utilize calcium. All these vitamins and minerals can be obtained in the right quality and quantity from food and sunlight.
– The typical western diet of refined foods, meat, dairy products, eggs, sugar, alcohol and coffee does not adequately supply our vitamin and mineral needs. Our weight-reducing diets are deficient in many essential nutrients.
– Meat, like dairy products, has too much protein for the body to utilize efficiently. When we eat meat, an acid, high-phosphorus condition is created in the blood. Phosphorus is absorbed more easily than calcium, has a see-saw relationship with calcium and forces calcium down when it goes up, and can accelerate bone loss. The acid condition can dissolve calcium from the bones. If a high protein diet is consumed, it is impossible to maintain a positive calcium balance regardless of the amount of calcium taken in. Iron and zinc are also lost when a high protein diet is eaten. Some researchers believe zinc to be even more important than calcium in maintaining strong bones. Other foods high in phosphorus and best avoided are: sodas, instant soups, some gelatins, snacks (like pork rinds), baking powder and dish detergent (if not thoroughly rinsed off dishes can also be a source of excess phosphorous.)
– Too much salt interferes with calcium absorption and increases calcium loss.
– Sugars, including white sugar, syrups, honey and malt cause calcium to be lost.
– Caffeine and other methylxanthines, as found in coffee, colas, tea and chocolate, blocks calcium absorption from our food. Drinking 2-4 cups of coffee a day for a 15 year period can set the stage for developing osteoporosis. The same is true for alcoholic drinks. Tobacco has been found to alter natural estrogen metabolism and accelerate bone loss. Smoking causes about 1% bone calcium loss per year occurring from less than a pack per day. Cancer, heart disease, and diabetes can all promote osteoporosis, and all have dietary causes.

TREATMENT
– Lifestyle and diet according to the HEALTH RECOVERY PLAN >
Researchers have established that proper nutrition and weight-bearing exercises are successful in preventing osteoporosis and sometimes in reversing it.
– Treat MENOPAUSE >
– In majority of cases osteoporosis is closely linked to low oestrogen, hormonal imbalance and menopause. For this reason it is very important to normalise oestrogen and other hormones. For a few years I have been recommanding Menovital (HealthAid) because I like its ingredients and quality and many ladies told me it usually gives best results in regulating estrogen and removing unpleasant symptoms associated with menopause.
– Silica: There is no question that silica plays a very important role in bone formation and in bone health, and like Vitamin K2 and Vitamin D, Silica seems to be much more important for strong bones than Calcium. Professor Kervran proved that 14 atoms of silica and 6 atoms of carbon make 20 atoms of calcium. He gave chickens silica and no calcium and they produced solid, hard calcium eggshells. When he took the silica out of their diet, the eggshells were soft and couldn’t form the calcium.
– Calcium intake is promoted by the dairy industry as the primary factor in osteoporosis. Advertising campaigns have been designed to persuade us that taking calcium supplements and drinking and eating dairy products are absolutely necessary for bone growth. But research has proven that supplementing calcium does not promote new bone growth. Calcium carbonate supplements have been found to actually suppress bone growth.
In studies of the Chinese, it has been found that although the Chinese consume half the amount of calcium Americans do, osteoporosis is uncommon in China. Most Chinese people eat no dairy products, 1/3 the amount of fat and twice the complex carbohydrates as Americans. They eat 20% more calories, but Americans are 25% more overweight. The average Chinese diet consists of 7% protein from animals; Americans consume 70% protein from animals!
– Oestrogen is often prescribed to prevent osteoporosis but it greatly increase the risk of heart disease, endometriosis, breast cancer and other cancers. Because of these side effects of estrogen, physicians have tried using progesterone along with estrogen in attempt to prevent these problems. Unfortunately, progesterone carries risks of gall bladder disease, certain cancers, hypertension and heart disease.
– Fluoride is another drug prescribed to slow down bone loss. But any beneficial effects are accompanied by serious side effects in the stomach and joints. Furthermore, broken bones have been found to increase among patients treated with fluoride.
– Exercise every day. Fast walking outside is one of the best types of physical activity. Exercise is one of the best ways to strengthen bones. Physical activity causes that our body needs strong bones so bone cells open the door for calcium and strengthen themselves. In long-term studies, researchers have found that regular participation in weight-bearing exercise, leads to a significant increase in bone mineral content. In many instances, osteoporosis can be improved. The more active we are, the thicker our bones grow. There is a connection between muscle strength and bone density. When we move our muscles, the pull of muscles on bones and the jolting of exercise, encourages the bones to absorb more calcium. Exercise, to be effective in maintaining bone density and overall fitness, needs to be undertaken at all stages of life; from childhood on through advancing age. People who are just beginning to show signs of osteoporosis can prevent its progression by adding an exercise program to their daily schedule. This is as important as beginning a new eating program. Healing is slow and gradual, and takes place over the course of many months and possibly years. Once osteoporosis has developed to the point of a high fracture rate, extreme care must be taken when initiating exercise, because even small body stresses can cause fractures. Another concern is exercising too much. Excessive exercise, such as the kind of training needed to participate in marathon running or professional dancing, can cause painful heels, shin splints, headaches, blood in the urine, irregular or stopped menstruation. It can also cause bones to become thin and weak. This type of osteoporosis has been found in women as young as 25 years. Moderation and enjoyment are the keys to a beneficial exercise program. The amount of exercise will vary with each person depending on the overall health. Walking is good for a start, then aerobics, cycling, and purposeful labour are good weight-bearing activities. Swimming is not a good weight-bearing exercise because water reduces the effect of gravity and there is less weight demand put on muscles and bones. This kind of exercise is good for advanced osteoporosis. Stretching is also good for muscles and bones and helps prevent humpback. Start slowly and increase your time weekly, until you’re exercising two hours per day. Then decide if you want to add more vigorous exercise, depending on your condition. Books in libraries and book stores teach different types of exercise, from easy stretching, to the most demanding labour. Warm up slowly each exercise period or you can get muscle and tendon strains. Cool down slowly for a few minutes before sitting or lying down to prevent heart and lung congestion.
– Avoid or greatly reduce consumption of animal protein (dairy, meat, etc.). In Africa where intake of animal protein is very low women do not suffer from osteoporosis. In America and Scandinavian countries calcium intake and dairy consumption is the highest in the he world and the prevalence of osteoporosis and hip fractures is the highest too! Experiments by Prof Walter Veith demonstrated that the more dairy protein animals were given with food the weaker their bones. Plant protein from soy and beans did not produce harmful effect.
– Go on unrefined plant-based diet. Osteoporosis is to a great degree a total dietary problem, not merely a calcium problem. Our bodies can adapt to a reduction in calcium intake by increasing the efficiency of intestinal calcium absorption. Usually only about 30% of the calcium we eat is absorbed. But when needed we can double or nearly triple the absorption. If we choose to eat a balanced vegetarian diet, we can prevent, and in many instances partially reverse osteoporosis. Studies done to compare bone density in meat eaters and vegetarians, found that vegetarians had greater bone densities than meat eaters, even though the quantity of bone calcium was lower in the vegetarians. Those vegetarians who reach approximately 69 years of age, appear to suffer no further decline in bone density, whereas in meat eaters, bone loss continues.
Healthful Eating Habits: Most mistakenly believe that the loss of natural estrogen during menopause, either natural menopause or surgical, is the most important factor leading to osteoporosis. Against the estrogen theory being an important factor is the generally observed development of strong bones in little girls who have even less estrogen than post-menopausal women. But, if for many years a woman has been eating and drinking foods that contribute to bone loss, by the time estrogen production declines, her bones have already been weakened by a poor diet. Whereas, if a woman has been eating healthful, whole vegetarian foods, staying away from harmful foods, and engaging in regular exercise, by the time she reaches menopause, her bones are most likely in a strong state of health. Even when a radiologist judges a vegetarian woman’s bones to be thin, she will rarely suffer a fracture.
There are certain plant foods that contain plant sterols similar to natural estrogen. We recommend emphasizing them in the diet. Whole, vegetarian foods are higher in carbohydrates and lower in protein than animal-based foods. The most favourable diet to prevent or treat osteoporosis is a totally vegetarian diet. The foods that are known to be rich in oestrogen-like sterols are: whole grains, seeds, soybeans, beans, peanuts, coconut, most nuts and seeds, beets, Brussels sprouts, carrots, corn, okra, radish greens, beans, barley and pea sprouts, yams, apples, cherries, figs, olives, plums, strawberries and herbs like alfalfa, anise seed, garlic, liquorice root, oregano, parsley, and sage.
– Avoid drugs as much as possible as many cause osteoporosis, especially aluminium antacids
– Treat anorexia nervosa and bulimia, diabetes, rheumatoid arthritis
– Avoid acid forming foods such as vinegar, animal products; baking powder; and foods high in sugar, salt or fat
– Boxed, canned, and frozen foods should be avoided when fresh food is available, as they are often deficient in nutrients and loaded with bone-robbing salt, fat or sugar. There are many cookbooks available today to teach you how to prepare natural foods in a variety of interesting, delicious ways.
– Plant foods supplying calcium in adequate quantities so that questionable dairy products or calcium supplements will be unnecessary include most seeds; greens like spinach, kale, mustard, cauliflower, broccoli, Brussels sprouts and celery; carrots; green peas; green snap beans; oatmeal; cream of wheat; cashews; almonds; dried fruits; lentils; lima beans; soybeans and soybean products like tofu.
Green and yellow vegetable consumption is effective for maintaining bone mass in young women >
Soy product consumption is inversely associated with the risk for hip fracture in men and women >
Dried plum improves bone mineral density in postmenopausal women >
– Since every plant food contains protein, human needs are provided by a vegetarian diet. Fresh cabbage has more protein per unit volume than whole milk. Rice, corn, fruit, wheat flour, dried beans and peas supply enough usable protein to safely maintain our health. By eating a variety of whole foods, all vitamin and mineral needs are met, without burdening the body with toxic excess that creates disease.
VITAMIN K – MOST IMPORTANT NUTRIENT FOR STRONG BONES
Together with vitamin D vitamin K make sure that the calcium in your body is stored in bones and used to make them strong and healthy. Without these two vitamins calcium cannot be stored in bones! For this reason calcium supplement should always be taken with vitamin D3 and K2 MK7!
Take vitamins D3 and K2 to ensure proper assimilation of the calcium into the bones to maintain bone strength so it doesn´t end up in places that will cause pain and inflammation.
Vitamin K is required for the production (in osteoblasts) and proper function of enzyme osteocalcin required for proper bone-forming process. Vitamin K2 has been found to be far more effective in this process than Vitamin K1.
Inadequate K2 inhibits osteocalcin production and reduces calcium flow into bone tissue. This leads to reduced bone mass.
Japanese trials have demonstrated that vitamin K2 can reverse bone loss and increases bone mass in people with Osteoporosis. The evidence shows that Vitamin K2 supplementation produces a 60% reduction in vertebral fractures and an 80% reduction in hip and other non-vertebral fractures.
A two-year study found that 45 mg/day of vitamin K2 reduced the incidence of vertebral (spine) fractures by 52% in 120 patients with osteoporosis, compared with patients who did not receive this nutrient.
For reducing fractures, the research overwhelmingly supports vitamin K2 in the form of MK4 and very high dosages of 45 mg/day. Numerous clinical trials using 45 mg per day of MK4 indicate that only this mega dose of MK4 taken daily may decrease fractures more than 80%. For instance, a 2006 study concluded that 45 mg of MK4 can decrease vertebral fractures by approximately 60%, hip fracture by 70%, and all non-vertebral fractures (ribs & wrist) by 80%.
By now only MK4 has demonstrated the ability to decrease fractures. MK7 has never been shown in any studies to reduce fractures.
VITAMIN K PREVENTS HARMFUL EFFECTS OF CALCIUM
Never take calcium supplements without vitamin K2 MK7, D3 and good magnesium, because if you are deficient in these nutrients (and almost all people today are), calcium you get from supplements, hard water or food, instead of strengthening your bones will be deposited in pineal gland (leading to its calcification), kidneys (causing kidney stones) and arteries (causing their hardening and leading to heart attacks and strokes).
– Vitamin K2 (must be MK2 from fermented Natto). According to Dr Mercola, “Vitamin K is the missing nutrient to blame for heart attacks and osteoporosis.”
CALCIUM CITRATE NOT CARBONATE
– Calcium (only citrate as it is organic) never carbonate or bicarbonate unless it is combined with calcium citrate and other vitamins and minerals necessary to maintain healthy bones. Calcium supplements must be always taken with vitamin D3, Magnesium, Boron, Zinc and K2. All these ingredients are present in Osteozin (HealthAid).
VITAMIN D
– Vitamin D3 – 20,000 IU a day with meal for one or two months and 5,000 IU a day after that. Vitamin D deficiency plays important role in the development of osteoporosis. It is essential in helping your body to properly absorb and use calcium which helps to keep spine and bones strong. Without vitamin D, our body begins to robe the spine of calcium. Since vitamin D supplements lead to magnesium deficiency, and because according to recent studies almost every in the UK person is now deficient not only in vitamin D but also magnesium, you must take 400 to 800mg of good quality magnesium every day. The most important way of obtaining vitamin D is of course through regular sun exposures during summer time between 10am and 2pm. Unfortunately, since in the UK almost every person is deficient in vitamin D the only solution seems to be supplementation. Read more about vitamin D >
Vitamin D requires magnesium and vitamin k2 for absorption and leads to magnesium deficiency. Therefore, the more vitamin D taken the more magnesium supplements are required! Never take calcium supplements without vitamin D:
Calcium supplementation (without vitamin D) is associated with increased risk of bone fracture >
EXCESS SUPPLEMENTAL VITAMIN D & CALCIFICATION
Vitamin K2 should be always taken with Vitamin D supplements, especially when high doses of vitamin D are taken for a long time. Taking vitamin K2 will prevent calcification of blood vessels or kidney stones caused by long-term overdosing of vitamin D.
I myself often recommend vitamin D3 supplementation due to the huge deficiency but it should always be accompanied by proper intake of vitamin K2 and magnesium.
The main consequence of vitamin D toxicity is a build-up of calcium in the blood (hypercalcemia), which may cause weakness, nausea and vomiting, frequent urination, etc. These symptoms might progress to arterial calcification, bone pain and the formation of calcium stones in kidneys.
Taking over 50,000 international units (IU) a day of vitamin D for longer time such as several months may lead to toxicity. Such mega doses can be taken but only for shorter periods of time (1 to 3 months) followed by the reduction of the dosage to 5-10,000 IU per day and always with 100-200mcg K2 and 2 times a day 400-800mg of Magnesium (such as citrate).
Treatment of Vitamin D toxicity includes stopping vitamin D intake and restricting dietary calcium until recovery.
MAGNESIUM
– Deficiency of Magnesium contributes to osteoporosis. Take 800mg or 2 x 400mg of well-absorbed magnesium citrate between meals with water. MagCitra is an excellent supplement as it is high in elemental magnesium citrate. Also remember to take magnesium whenever you use vitamin D supplements as it leads to magnesium deficiency! The more vitamin D3 you take the higher doses of magnesium you need.
OTHER SUPPLEMENTS
– Boron
– Zinc
– Regular sunbathing (if possible) as it produces vitamin D.
– Hot and cold alternative showers
– Avoid sugar, fructose, glucose, coffee, tea, and other stimulants.
– Good quality Omega 3 (high in EPA) on a daily basis.
– Chlorella: 3 tabl (or 1 teaspoon of powder) 30 min before breakfast and 1 tabl 30 min before lunch with vegetable juice or water. Every day increase dosage by 1 tabl until 10 tabl (or 1 heaped tablespoon) 30 min before breakfast and 10 tabl 30 min before lunch (always with 2-3 glasses of water or vegetable juice).
Chlorella, Spirulina and seaweeds have been reported to help re-mineralize bones. It was once thought that bones could not be recalcified, but it is now recognized that sometimes calcium can be replaced in the bones. Starting with a mild variety of seaweed, like Arame, is a good way to begin to get used to this new taste. Nori comes in dark green dried sheets. Seaweeds can be purchased in health food stores or Oriental groceries. Most have to be soaked and cooked, but Dulse and Seapalm can be eaten right out of the bag. Nori can also be eaten straight from the bag or lightly toasted until it turns a beautiful green. Vegetables can be added to a seaweed dish or seaweed can be added to cooking beans, greens or pasta or crumbled over cooked dishes. Care should be taken to rinse the extra salt off the saltier varieties.
Chlorella is regarded as the best natural energy booster, detoxifier, pain reliever, and regenerating agent. It is a highest source of nucleic acids RNA and DNA which are capable of repairing damaged DNA. Chlorella together with other supplements and herbal remedies will slowly rebuild the annulus fibrosus which is the key cause of the herniated disc. Since chlorella is 10 times higher in chlorophyll than green leafy vegetables it is best possible oxygen pump in human body. In case of bulging disc it is extremely important as one of the main problems about discs healing is that they do not receive proper supply of oxygen. You can also increase the oxygen level through walking. Read more about amazing healing properties of Chlorella >
 – Excellent and very effective Clean Greens (Pukka) or Raw Reserve (Amazing Grass): 1 teaspoon of the powder 30 min before breakfast with vegetable juice or water and 1 teaspoon 30 min before lunch. It can be taken together with chlorella.
– Excellent and very effective Clean Greens (Pukka) or Raw Reserve (Amazing Grass): 1 teaspoon of the powder 30 min before breakfast with vegetable juice or water and 1 teaspoon 30 min before lunch. It can be taken together with chlorella.
Clean Greens is one of the most powerful remedies I know as many of our customers told me how effective this formula was in dealing with inflammations, back pains, chronic fatigue, diabetes, cancer, gastrointestinal problems, liver and kidneys problems, weak immune system, etc. It consists of organic blend of 11 super-rich mostly freeze-dried green super foods including Wheat Grass Juice (30 times stronger than regular juice!), Nettle, Chlorella, Spirulina, Kale Sprouts, Seagreens, freshwater plants and digestive herbs. Made with some of nature’s finest herbs, grown in fertile organic soils it captures the incredible essence of nature’s bounty.
– Drink only distilled water > and avoid hard water (high in calcium) because it contains inorganic calcium carbonate which is harmful and contributes to arthritis, kidney stones, constipation and hardens arteries. Add a little bit of fresh lemon juice to your distilled water to make it more alkaline and tastier.
Read a fascinating article about WATER >
– Free, Inspired, Life-Transforming Book!
– Can Christ Return in 2027
ARTICLES (TRANSCRIPTS) BY MICHAEL GREGER M.D.
Is Milk Good for Our Bones?
Plant-based sources of calcium are superior to animal-based sources (kale and broccoli absorbed nearly twice as well as the calcium in cow’s milk). A comparison of the bone mineral density of vegans to omnivores found that though omnivores have more than twice as much calcium intake due to dairy consumption, both had the same bone density. Though dietary intake studies show that those eating vegan tend to be deficient in calcium as well as two other nutrients, those eating conventional diets also tend to be deficient in calcium (and 6 other nutrients). Soymilk can provide the same amount of calcium as cow’s milk as long as the soymilk is shaken. There does not appear to be credence to the theory that protein intake in is bad for bones, but AGEs and coffee consumption may have adverse effects on bone health.
Milk is touted to build strong bones, but a compilation of all the best studies found no association between milk consumption and hip fracture risk, so drinking milk as an adult might not help bones. But what about in adolescence? Harvard researchers decided to put it to the test. Studies have shown that greater milk consumption during childhood and adolescence contributes to peak bone mass, and is therefore expected to help avoid osteoporosis and bone fractures in later life. But that’s not what they found. Milk consumption during teenage years was not associated with a lower risk of hip fracture, and, if anything, milk consumption was associated with a borderline increase in fracture risk in men. It appears that the extra boost in total body bone mineral density you get from getting extra calcium is lost within a few years, even if you keep the calcium supplementation up. This suggests a partial explanation for the long-standing enigma that hip fracture rates are highest in populations with the greatest milk consumption. Maybe an explanation why they’re not lower, but why would they be higher? This enigma irked a Swedish research team, puzzled because studies again and again had shown a tendency of a higher risk of fracture with a higher intake of milk. Well, there is a rare birth defect called galactosemia, where babies are born without the enzymes needed to detoxify the galactose found in milk, so they end up with elevated levels of galactose in their blood, which can cause bone loss even as kids. So maybe, the Swedish researchers figured, even in normal people who can detoxify the stuff, it might not be good for the bones to be drinking it every day. And galactose doesn’t just hurt the bones. That’s what scientists use to cause premature aging in lab animals They slip them a little galactose and you can shorten their lifespan, cause oxidative stress, inflammation, brain degeneration, just with the equivalent of one to two glasses of milk’s worth of galactose a day. We’re not rats, though—but given the high amount of galactose in milk, recommendations to increase milk intake for prevention of fractures could be a conceivable contradiction. So they decided to put it to the test, looking at milk intake and mortality, as well as fracture risk, to test their theory. A hundred thousand men and women followed for up to 20 years; what did they find? Milk-drinking women had higher rates of death, more heart disease, and significantly more cancer for each glass of milk. Three glasses a day was associated with nearly twice the risk of death. And they had significantly more bone and hip fractures too. Men in a separate study also had a higher rate of death with higher milk consumption, but at least they didn’t have higher fracture rates. So a dose-dependent higher rate of both mortality and fracture in women, and a higher rate of mortality in men with milk intake, but the opposite for other dairy products like soured milk and yogurt, which would go along with the galactose theory, since bacteria can ferment away some of the lactose. To prove it though, we need a randomized controlled trial to examine the effect of milk intake on mortality and fractures. As the accompanying editorial pointed out, we better figure this out soon, as milk consumption is on the rise around the world.
Almonds for Osteoporosis
Currently, an estimated ten million Americans suffer from osteoporosis, causing more than a million fractures, including hundreds of thousands of hip fractures, a common reason people end up in nursing homes. Many older women say they’d rather be dead than break their hip and end up in a home. Bone is a dynamic, living organ that is constantly renewed through a process of remodelling and modeling involving bone breakdown by cells that eat bone, called osteoclasts, and bone formation by cells that build bone, called osteoblasts. Osteoporosis is caused by an imbalance between bone loss and bone gain, most often related to hormonal changes that occur during menopause. Is there anything we can do to help tip the balance back in bone’s favour? There are a number of specific compounds in plant foods that look promising, but that’s based on in vitro studies like this, where they basically just drip some plant compound on bone cells in a petri dish and see a boost in bone builder cells, or a drop in bone eater cells. But no matter how much people like cranberry sauce, they’re not injecting it into their veins. For phytonutrients to reach the bone, they first have to get absorbed from the digestive tract into our bloodstream and make it past the liver before they can circulate to our skeleton. So, what we would need is a so-called ex vivo study, where you take people, feed them a food—or not—and then draw their blood a few hours later and then drip their blood onto bone cells and see if there’s any difference. But nothing like that had ever been attempted until this study. Normally, I’m not impressed with studies funded by marketing boards, which pay for studies like this that found that eating almonds improved cycling distance and athletic performance… compared to cookies. But this study was brilliant, not surprisingly, given it was performed in the world-famous lab of Dr. David Jenkins. There was a population study that suggested that eating almonds could protect against osteoporosis; so, they could have just dripped some almond extract on bone cells, but that’s not testing the whole food. Instead you could treat bone cells with the blood obtained from donors fed the whole food to directly test the effects of these foods at the cellular level. So, they exposed human osteoclasts, the bone eaters, to blood obtained before and four hours after eating a handful of almonds. But wait a second, before I get to the results, if you ate a handful of almonds every day, wouldn’t you gain weight—that’s almost 200 calories? Let’s find out. If you add a handful or a handful and a half—like 35 almonds in addition to women’s regular diet as a mid-morning snack, and tell them to eat as much as they want for lunch and supper that day, people eat less; in fact so much less, they cancel out the nut calories. In this study, they all had the same breakfast, then zero, 173 or 259 calories worth of almonds as a snack, then ate as much lunch as they wanted, but the nuts appeared to be so satiating that they ate less for lunch or dinner such that, at the end of the day, there was no significant difference in total caloric intake between any of the three groups. Part of the reason we don’t tend to gain weight adding nuts to our diet may be because we end up flushing nearly a third of the calories down the toilet, because we just don’t chew well enough. This is why we think there’s so much less fat in our bloodstream after eating whole almonds compared to the same amount of almond oil taken out of the nuts. So anyway, they wanted to see if they could suppress the activity of the cells that eat away our bones. And they found that blood serum obtained following the consumption of an almond meal inhibits human osteoclast formation, function, and gene expression, providing direct evidence to support the association between regular almond consumption and a reduced risk of developing osteoporosis. They also tried before and after eating other meals, rice or potatoes, to make sure there wasn’t just some effect of eating in general and no, the protective effect did appear specific to the almonds.
Are Calcium Supplements Effective?
There has been an assumption for decades that as a natural element, calcium supplements must intrinsically be safe, but calcium supplementation is neither natural nor risk-free. But, the same could be said for every medication on the planet. Yet, doctors continue to write billions of prescriptions for drugs every year because the hope at least is that the benefits outweigh the risks. So, what about the benefits of calcium supplements. Yes, heart attacks and strokes can be devastating, but so can hip fractures. The risk of dying shoots up in the months following a hip fracture. About one in five women don’t last a year after a hip fracture, and it may be even worse for men, on average apparently cutting one’s lifespan short by four or five years. And, unfortunately these dismal statistics don’t seem to be getting much better. So, even if calcium supplements caused a few heart attacks and strokes, if they prevented many more hip fractures, then it might result in a favourable risk-benefit ratio. So, how effective are calcium supplements in preventing hip fractures? We’ve known that milk intake doesn’t appear to help, but maybe that’s because any potential benefit of the calcium in milk may be overshadowed by the increased risk of fracture and death associated with the galactose sugar in milk. So, what about just the calcium in a calcium supplement alone? Calcium intake in general does not seem to be related to hip fracture risk at all, and when people have been given calcium supplements, not only was there no reduction in hip fracture risk, an increased risk is possible. The randomized controlled trials suggested a 64% greater risk of hip fractures with calcium supplementation compared to just getting like a placebo sugar pill. Where then did we even get this idea that taking calcium supplements might help our bones? It was this influential study, in 1992 that found that a combination of vitamin D and calcium supplements could reduce hip fracture rates 43%. But, this was done on institutionalized women, like in a nursing home, who were vitamin D deficient. They weren’t getting sufficient sun exposure. And, so, if you’re vitamin D deficient and you take vitamin D and calcium, no surprise your bones get better, but for women living independently, out in the community, the latest official recommendations for calcium and vitamin D supplementation to prevent osteoporosis are unambiguous: Do not supplement. Why? Because in the absence of compelling evidence for benefit, taking supplements is not worth any risk, no matter how small. Now, this is not to say these supplements don’t play a role in treating osteoporosis, or that vitamin D supplements might not be good for other things, but if you’re just trying to prevent fractures, women living outside of institutions shouldn’t take them and perhaps even in institutions. In this study, instead of giving nursing home residents vitamin D and calcium supplements, they randomized them to sunlight exposure and calcium supplements, and those that got the calcium pills had significantly increased mortality, lived shorter lives than the sunshine only group. Although calcium supplements don’t appear to prevent hip fractures, they may reduce overall fracture risk by like 10%. So, here’s how the risk-benefit shakes out. If a thousand people took calcium supplements for five years, we would expect 14 excess heart attacks, meaning 14 people would have a heart attack that would not have had a heart attack if they hadn’t started the calcium supplements. So, they were effectively going to the store and buying something that gave them a heart attack, plus ten strokes that otherwise would not have happened, and 13 deaths—people who would have been alive had they not started the supplements. But, that’s all balanced against the 26 fractures that would have been prevented. Now, it’s no fun falling down and breaking your wrist or something, but I think most people would look at risk benefit analysis and conclude that calcium supplements are doing more harm than good. Given these findings, the use of these supplements should be discouraged, and individuals advised to obtain calcium from their diet instead. Calcium supplements have been associated with elevated risk of myocardial infarction (heart attacks), whereas dietary calcium intake has not. How much calcium should we shoot for? Interestingly, unlike most other nutrients, there’s no international consensus. For example, in the UK, the recommendation for adults is 700 mg a day, but across the pond in the US, it’s up to 1,200 a day. Whenever I see that kind of huge discrepancy between government panels, I immediately think scientific uncertainty, political manoeuvrings, or both.
Newer data, based on calcium balance studies in which researchers make detailed measurements of the calcium going in and out of people, suggest that the calcium requirement for men and women is lower than previously estimated. They found calcium balance was highly resistant to change across a broad range of intakes, meaning our body is not stupid. If we eat less calcium, our body absorbs more and excretes less, and if we eat more calcium, we absorb less and excrete more to stay in balance. Therefore, current evidence suggests that dietary calcium intake is not something most people need to worry about.
This may explain why in most studies, no relationship was found between calcium intake and bone loss anywhere in the skeleton, because the body just kind of takes care of it. Don’t push it too far, though. Once you get down to just a few hundred milligrams a day, you may get significantly more bone loss. Though there may not be great evidence to support the U.S. recommendations, the UK may have the right idea shooting for between 500 and 1,000 mg a day from dietary sources unless you’ve had gastric bypass surgery or something and need to take supplements. For most people, though, calcium supplements cannot be considered safe or effective for preventing bone fractures.
Phytates for the Prevention of Osteoporosis
Health authorities from all over the world universally recommend increasing consumption of whole grains and legumes—beans, split peas, chickpeas, and lentils—for health promotion. But what about the phytates? Phytate is a naturally occurring compound found in all plant seeds, meaning all beans, grains, nuts, and seeds, which over the decades has been badly maligned as a mineral absorption inhibitor. That’s why, for example, you hear advice to roast, sprout, or soak your nuts—to get rid of the phytates so we can absorb more minerals like calcium. The concern about phytates and bone health arose from a series of laboratory experiments performed on puppies published in 1949, suggesting high phytate diets have a bone softening and anti-calcifying effect. Subsequent studies on rats, in which they fed them the equivalent of 10 loaves of bread a day, confirmed phytate’s status as a so-called anti-nutrient. But more recently, in the light of actual human data, phytate’s image has undergone a makeover. If you put people on a high phytate diet and measure their calcium balance, their bodies appear to become accustomed to the extra phytate over time and it all worked out, but this study was done on only 3 people. So I was glad to see this study published, which asked the simple question, do people who avoid high phytate foods—legumes, nuts, and whole grains—have better bone mineral density? No, in fact just the opposite. Those that consumed more high-phytate foods had stronger bones, as measured in the heel, spine, and hip. The researchers conclude that dietary phytate consumption had protective effects against osteoporosis and that low phytate consumption should be considered an osteoporosis risk factor. This is consistent, with reports that phytate can inhibit the dissolution of bone similar to anti-osteoporosis drugs like Fosamax. A follow-up study found the same thing: improved bone density in those that consumed the most phytates, but this is the most convincing study to date, actually measuring phytate levels flowing through women’s bodies and following bone mass over time. And women with the highest phytate levels had the lowest levels of bone loss in the spine, and the hip, and so no surprise that those who ate the most phytates were estimated to have a significantly lower risk of major fracture, and lower risk of hip fracture specifically. This is thought to be in part because phytates help block the formation of bone-eating cells, and their bone-eating activity. You can see how much more bone is eaten away in the nonphytate group on the left. Now the drug Fosamax can have a similar beneficial effect, but phytates don’t have the side effects associated with bisphosphonates, like osteonecrosis. There’s a rare side effect associated with this class of drugs called osteonecrosis of the jaw. The whole reason people take these drugs is to protect their bones, but by doing so, also risk rotting them away.
Alkaline Diets, Animal Protein, & Calcium Loss
For most of the last century, a prevailing theory within the field of nutrition was that by eating acid-forming foods such as meat we were, in essence, at risk of peeing our bones down the toilet. And no wonder! Experiments dating back to 1920 showed over and over that if you add meat to the diet you get a big spike in the amount of calcium being lost in the urine. And this made total sense. We had known since 1912 that meat was acid-forming within the body, and how do you buffer acid? What are in antacid pills, anti-acid pills like tums? Calcium. Meat and eggs have a lot of sulphur-containing amino acids, 2-5 times more than grains and beans) that are metabolized into sulphuric acid, which the body buffers with calcium. That’s why the antacids like Tums are made out of calcium, calcium compounds can buffer acid. And where is calcium stored in the body? The skeleton. So the thinking was that every time we ate a steak our body would pull calcium from our bones, bit by bit, and over time this could lead to osteoporosis. Based on 26 such studies, for every 40 grams of protein we add to our daily diet we pee out an extra 50mg of calcium. And look, we only have about 2 pounds of calcium in our skeleton, so the loss of 50 a day would mean losing close to 2% of our bone calcium every year. By the end of the 20th century, there was little doubt that acid-forming diets would dissolve our bones away. But if you actually look at all the studies done on protein intake and bone health, that’s not what you find. So, where’s the flaw in our logic? Meat leads to acid, which leads to calcium loss, which leads to bone loss, right? Well, it’s uncontroversial that protein results in greater calcium excretion, but we’ve just been assuming it’s coming from the bone—I mean where else could the extra calcium dumped in our urine be coming from but from our bones? This is the study that appeared to solve the mystery. An intrepid group of researchers tried feeding a group of volunteers radioactive calcium and then put them on a high protein diet. What happens when you put people on a high protein diet? The amount of calcium in their urine shoots up, and indeed that’s just what happened. But here’s the big question, was that extra calcium in their urine radioactive or not, and to everyone’s surprise? It was radioactive. Meaning, that the excess calcium in their urine was coming from their diet—remember they were feeding them radioactive calcium. So the excess calcium in their urine wasn’t coming from their bones, but from what they were eating. What seemed to be happening is that the excess protein consumption boosted calcium absorption, from down around 19% up to 26%. So all of a sudden there was all this extra calcium in the blood so presumably the kidneys are like “whoa what are we going to do with it all?” So they dump it into the urine. 90% of the extra calcium in the urine after eating a steak doesn’t appear to be coming from our bones but from our diet. We’re not sure why protein boosts calcium absorption. Maybe the protein increases the solubility of calcium by stimulating stomach acid production? Whatever the reason, yes, more calcium lost, but more calcium gained such that in the end most of that extra calcium is accounted for. So in effect more calcium is lost in the urine stream, but may be compensated by less loss of calcium through the fecal stream. This was repeated with even more extreme diets— an acid-forming five burgers a day worth of animal protein diet that limited fruits and vegetables versus an alkaline diet emphasizing fruits and vegetables. More calcium in the urine on burgers, but significantly greater calcium absorption such that at the end it was pretty much a wash. Other studies have also since supported this interpretation. Here’s an ingenious one. Feed people a high animal protein diet, but with an alkali salt to neutralize the acid. The old thinking would predict that then there would be no calcium loss since there is no excess acid to buffer, but no, even though the acid load was neutralized there was still the excess urinary calcium, consistent with the radioactive isotope study, “challenging the long-standing dogma that animal protein consumption results in an acidosis that promotes the increased excretion of calcium…. So if our body isn’t buffering the acid formed from our diet with our bones, how is it neutralizing the acid? Maybe with our muscles–alkaline diets may protect our muscle mass—all covered in my next video, entitled Testing Your Diet with Pee and Purple Cabbage—stay tuned!
READ ALSO:

Share this article!
REFERENCES
Carper, Jean, “Food Pharmacy,” The Atlanta Journal and Constitution, 1990
Glassburn, Vicki, Who Killed Candida?, Teach Services, 1991
Palm Beach Post, 1990
Yeater, Rachel A. PhD; Martin,Bruce R. PhD, “Senile Osteoporosis,” Post Graduate Medicine, 1984
Gerber, N.J., Rey, B., “Can Exercise Prevent Osteoporosis?,” British Journal of Rheumatology, 1991
Oestreicher, Annette, Hippocrates, 1991
Childers, Norman, Prof., Letter to Arthur Brown, Sec., Dept. of Agriculture, 1986
Stevenson, John C. MB, MRCP, “Pathogenesis, Prevention, and Treatment of Osteoporosis,” Obstetrics and Gynecology, 1990
Cooper, C.; Wickham, C.; Coggon, D.; British Journal of Industrial Medicine, 1990
Grant, Alexander, Dr., Health Gazette, 1989
Rheumatology News, 1984
Brody, Jane, “China Study Challenges Diet Myths,” The Atlanta Journal and Constitution, 1990
Ellis, Holesh, and Ellis, “Incidence of Osteoporosis in Vegetarians and Omnivores”, Journal of Clinical Nutrition, 1972
Thrash, Calvin, Dr.; Thrash, Agatha, Dr., Nutrition For Vegetarians, Seale, AL: New Lifestyle Books, 1982
Dawson-Hughes, Bess, “Calcium Supplementation and Bone Loss”, American Journal of Clinical Nutrition, 1991
“Premenopausal Bone Mass Related to Physical Activity,” Archives of Internal Medicine, 1988
Mundy, Gregory R., MD, “Identifying Mechanisms for Increasing Bone Mass,” The Journal of NIH Research, 1989
Kendall, Lee G., Jr., MD, “Postmenopausal Osteoporosis,” Arthritis Today, 1986
Any information or product suggested on this website is not intended to diagnose, treat, cure or prevent any medical condition. Never disregard medical advice or delay in seeking it because of something you have read on this website. Consult your primary healthcare physician before using any supplements or making any changes to your regime.
