AUTOIMMUNE DISEASES
Written by Slawomir Gromadzki (“Swavak”), MPH
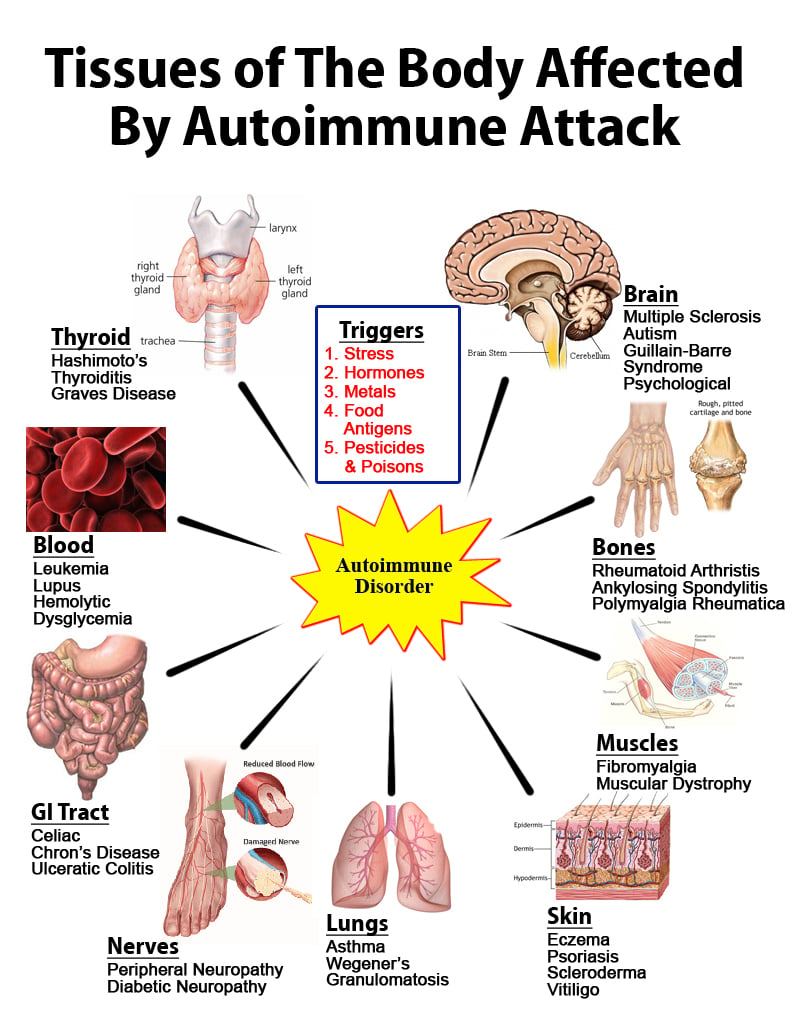
Autoimmune diseases cause immense suffering and pain. In people who suffer from various autoimmune conditions, the immune system produces antibodies that attack the body’s own tissues. There are about 160 different individual autoimmune diseases or over 80 types categorized according to different parts of the body that are affected.
KEY CAUSES
– Vitamin D3 deficiency. There is a growing amount of research which suggests that a lack of vitamin D could be an important factor in causing all 160 autoimmune diseases. Almost every person in England is deficient in vitamin D which is very important also for human nervous and immune system.
In his bestselling book “China Study” Prof Colin Campbell wrote that, “Autoimmune diseases in general become more common the greater the distance from the equator. This phenomenon has been known since 1922.” This statement leads us to a simple conclusion that all autoimmune diseases have a lot to do with the vitamin D (“sun vitamin”) deficiency, as well as the modern unhealthy lifestyle of North America or Europe. Read more about vitamin D >
– Iodine deficiency (due to soil depletion there is not enough iodine in food). The thyroid gland requires iodine to produce its hormones. In fact, it is believed that iodine’s only role in the body is to make thyroid hormones. However, it is important to know that not only too little of iodine can cause impaired thyroid function, but also too much can interfere with the gland’s ability to produce its hormones. Unfortunately there is disagreement with regards to sufficient iodine daily requirements. Some maintain that the dosage range for iodine supplementation should be 300-400 mcg daily but others suggest that it is way too low.
– Magnesium, Zinc, and Selenium deficiency.

– Toxins: Mercury (from dental fillings, tap water, fish, flu shots, etc.) lead, fluoride, and other toxins.
– Food intolerances: Gluten and A1 Casein intolerance.
– Hormonal Imbalances: Too much Cortisol (from stress).
– Stress, anxiety and depression. A number of published papers have shown that stress and negative emotions contribute to all autoimmune diseases.

– Consumption of trans fats, margarine and bad oils (high in pro-inflammatory omega 6) and deficiency of omega 3 healthy fats high in foods such as Flax seed, Chia seed, etc..
– Bad lifestyle, unhealthy diet high in sugar, processed refined foods, nutritional deficiencies, artificial sweeteners, lack of exercise, stimulants, drugs, medication, and in particular excessive stress, depression and pessimism may lead to the oversensitivity of the immune system which changes its nature and starts attacking own body.
– Consumption of meat and dairy products (can trigger autoimmune response and causes hormonal imbalance), refined, junk and processed foods, refined sugar, white flour products, high glucose (high fructose) syrup, stimulants (including coffee, tea, green tea, cola, etc., nutritional deficiencies, white pasta, white rice, processed foods, stress, lack of exercise, etc.
– According to Dr Michael Greger, “Alkylphenols, flame-retardant chemicals, and perfluorochemicals, industrial pollutants found mostly in fish and meat, may be associated with thyroid disruption in young children and adults. Alpha-gal antibodies in meat may result in autoimmune conditions, including thyroid disorders. The artificial food colouring Red No. 3, too much seaweed of any type, and processed meat consumption may be linked to an increase risk of thyroid cancer. Poultry workers often have thyroid disorders.”
TREATMENT
Autoimmune conditions are treated with harmful medication, which have bad side effects. Fortunately it is possible to recover from autoimmune diseases by practicing healthy lifestyle and using natural remedies. The most important element of the treatment is implementing principles from the HEALTH RECOVERY PLAN >
NUTRITIONAL AND LIFESTYLE RECOMMENDATIONS
Autoimmune diseases can be reversed by practising the following guidelines:
– Avoid all animal foods including cheese, meat products, all dairy, stimulants (caffeine, alcohol, cigarettes, etc.).
– Go on vegan unrefined diet as it gives best results. Eat especially with lots of raw vegetables salads and raw vegetable juices.
– Proper stress control and positive thinking – extremely important!
– Eliminate all junk food, processed food, artificial sweeteners, trans fats, and anything with bad preservatives and chemical.
– Eating whole, unprocessed foods, and choosing as many organics as possible.
– Getting adequate sun exposure if possible (20 minutes a day during summer time between 10 am and 2 pm) to maintain vitamin D levels.
– Avoid gluten (wheat products, etc.). The molecular structure of thyroid tissue is almost identical to that of gluten and therefore the immune system may start sending antibodies not only against gluten proteins but against proteins found in different organs causing autoimmune diseases . In this way gluten can increase the autoimmune reaction. Many people with autoimmune diseases have an autoimmune reaction to gluten, and it usually goes unrecognised. Gluten can cause gastrointestinal system to malfunction, so foods aren’t completely digested. These food particles can then be absorbed into bloodstream where body misidentifies them as antigens and then produces antibodies against them.
– Avoid all dairy products as heated dairy protein (especially A1 casein) often irritates the immune system stimulating it to produce antibodies against different internal organs. The most common allergies and food intolerances today are from wheat and dairy products because of the hybridized proteins of gluten and a1 casein. These proteins can cause Leaky Gut Syndrome which leads to inflammation.
– Use glass bottles as Bisphenol A (BPA) which is found in plastic bottles and cans (they are lined up with plastic) disrupt endocrine system.
– Avoiding chlorine, fluoride (toothpastes with fluoride, etc.), and bromine as they also contribute to autoimmune diseases.
– Avoid hydrogenated fats and trans fats (margarines, doughnuts, cakes, etc.) and pro-inflammatory omega 6 fatty acids (soy oil, corn oil, sunflower oil, etc.).
Ray Peat Ph.D., a physiologist who has worked with progesterone and related hormones since 1968, says that the sudden surge of polyunsaturated oils into the food chain post World War II has caused many changes in hormones. He writes: “Their [polyunsaturated oils] best understood effect is their interference with the function of the thyroid gland. Unsaturated oils block thyroid hormone secretion, its movement in the circulatory system, and the response of tissues to the hormone. When the thyroid hormone is deficient, the body is generally exposed to increased levels of estrogen. The thyroid hormone is essential for making the ‘protective hormones’ progesterone and pregnenolone, so these hormones are lowered when anything interferes with the function of the thyroid. The thyroid hormone is required for using and eliminating cholesterol, so cholesterol is likely to be raised by anything that blocks the thyroid function.”
– Detoxifying body from heavy metals by using combination of: Chlorella, Milk Thistle, Turmeric, Cilantro.
– Remove any dental fillings containing mercury.
– Increasing intake of healthy fats such as raw coconut oil, coconut milk, avocado, chia seeds (soaked for at least 30 minutes or overnight), ground flaxseed, and hemp seeds as they will balance hormones. Coconut oil is one of the best foods for thyroid. Coconut oil is a saturated fat comprising medium chain triglycerides (MCTs), which are known to increase metabolism and promote weight loss. Coconut oil is very stable (shelf life of three to five years at room temperature), so body is much less burdened with oxidative stress than it is from many other vegetable oils.
– Increase consumption of vitamin A in the form of beta-carotene found in carrots, apricots, green leafy vegetables, etc.
– Eliminate stimulants (anything with caffeine or other similar harmful alkaloids: coffee, tea, green tea, mate, yerba mate, cola, chocolate, etc.).
– Exercise at least 30–60 minutes per day.
– Get enough sleep.
– Practice deep breathing.
– Address adrenal fatigue. A prolonged stress response can lead to adrenal exhaustion (also known as adrenal fatigue). Find out more about ADRENAL FATIGUE >
– Treat unresolved emotional issues as a source of stress. Autoimmune diseases reflect emotions and mental attitude. When people with autoimmune diseases make progress in treating unresolved emotional issues, their symptoms subside. Stress, anxiety or depression are often key culprits. It is important to identify the stressors and learn use ways such as prayer that can help to control stress and negative emotions.
– Read about the DEADLY CONSEQUENCES OF UNFORGIVINGNESS >
– Drink and use for cooking only distilled or at least filtered water. Not all water filters remove fluoride, so make sure the one you have does or use only distilled water (buy a water distiller). Taking chlorella and turmeric help to get rid of fluoride and heavy metals such as mercury.
HERBAL REMEDIES & SUPPLEMENTS
VITAMIN D3, ZINC & SELENIUM
Every day you need about 5000IU of Vitamin D3, up to 25mg of Zinc, and about 200-300mcg of Selenium as deficiency of all these three essential nutrients is rampant today and greatly contribute to the development and prevalence of autoimmune conditions including alopecia.
Vitamin D3, Zinc & Selenium are essential in preventing and treating autoimmune diseases as they all are known to stimulate suppressor T-cells of the immune system to prevent other white blood cells from attacking own body tissue!
– You must take Vitamin D3 because almost all patients suffering from autoimmune diseases patients are deficient in Vitamin D! While using vitamin D3 supplements always remember to take also well absorbed magnesium (such as citrate) as vitamin D supplements lead to magnesium deficiency over time. If you can’t afford higher doses take at least 5,000 IU of vitamin D3 a day with meal. But since deficiency of this vitamin is so widespread (especially in the UK) it would be better to take 20,000 to 30,000 IU a day with meals with appropriate doses of magnesium. Another requirement for proper absorption of vitamin D is 200 mcg of Vitamin K2 MK-7 (Derived from Natural Natto) a day. Read more about vitamin D >
– Magnesium citrate or another well absorbed magnesium: 2 times a day 200 mg between meals. The more vitamin D3 is used the more magnesium must be taken as D3 leads to magnesium deficiency. Autoimmune diseases including alopecia are often associated with low mood, depression and chronic stress. That is why magnesium is often recommended for people suffering from autoimmune conditions as magnesium enables us to control stress and is vital in our body for proper functioning of the nervous system and brain, promoting good mood and improves our sleep patterns. It’s been suggested that this is because Magnesium is involved in the synthesis and function of GABA and serotonin, neurotransmitters known to be most effective in calming the brain and promoting relaxation. That is why Dr. Berzin calls Magnesium “the nature’s anti-anxiety drug”.
– Apart from Ashwaganda you can use other herbal remedies and adaptogens such as Rhodiola and Tulsi (Holy Basil) tea or capsules.
– Unlike Echinacea that require caution for those with autoimmune conditions, Nigella sativa (Black Seed) seems to normalise human immune system supporting its function without stimulating autoimmune responses in people with oversensitive immune system. For this reason black seed oil is often recommended for people with various autoimmune problems. Due to its anti-inflammatory and immune-modulating properties black seed oil can be beneficial for people suffering from rheumatoid arthritis (>) and other autoimmune inflammatory conditions such as eczema or psoriasis.
There are numerous testimonials available online written by individuals who claim to be benefited by Nigella sativa.
– Boost Glutathione levels which is a most powerful of all antioxidants and strengthens the immune system and is one of the most effective remedies against autoimmune diseases. It increases body’s ability to modulate and regulate the immune system. It is also important to provide body with ingredients that increase glutathione production in the liver by taking turmeric, milk thistle, NAC (N-acetyl cysteine), bioactive whey protein, Glutamine, Alpha Lipoic Acid, bilberry, vitamin C, asparagus, broccoli, peaches, avocado, spinach, garlic, squash, grapefruit. Read more >
– Taking selenium supplements and increasing consumption of foods high in selenium (Brazil nuts, sunflower seeds, mushrooms, garlic, onions, etc.).
– Increase consumption of omega 3 fatty acids in the form of ground flax seeds, chia seeds. Omega 3s are the building blocks for hormones that control immune function and cell growth.
– Take good quality omega 3 fish oil supplements (HealthAid makes excellent omega 3 fish oil as it is molecularly distilled and therefore perfectly free from mercury and other contaminants >): 1000 mg 2 times a day with meals. I recommand this one also because it is high in both EPA and DHA (DHA omega 3 is more important in improving brain function while EPA in coping with inflammation). Research has confirmed that omega-3 fatty acids can improve the symptoms of ADHD more effectively than drugs.
If you don’t want to use a molecularly distilled omega 3 fish oil (such as the mentioned above one by HealthAid) it’s much better to use high in DHA omega 3 oil from algae (expensive) and not from fish as unlike fish oils, the algae-derived omega 3, is free from toxins that may be present in some low quality fish oils. In case you prefer to avoid swallowing gelatine capsule pierce or cut the omega 3 capsule and squeeze it into a meal or liquid.
– Vitamin B12: 1,000 to 2,000 mcg a day under the tongue (must be sublingual Methylcobalamin!). Many people with autoimmune diseases have low levels of this most important vitamin. Read a fascinating article on B12 >
– Zinc (helps produce thyroid hormone): 30 to 50mg a day after breakfast. Zinc plays also a role in regulating the immune system with implications in pathologies where zinc deficiency and inflammation are observed.
– Take good quality probiotic formulas as proper immune system function depends on a sufficient supply of healthy gut bacteria.
Autoimmune Disease Success Stories >
– Good quality Multivitamin-mineral formula or Vitamin B-complex: 1 tablet after breakfast. Please do not buy cheap formulas as their potency is very low and they contain only short list of inorganic ingredients. It must be a good quality formula such as Healthy Mega (HealthAid), VM75 (Solgar) or Special Two (NOW Foods) which are an excellent multi-vitamin and mineral formulas fortified with alfalfa powder, rutin, citrus bioflavonoids, bromelain, herbs, digestive enzymes and many other super nutrients. If your diet is very healthy and you stay away from refined foods, sugar and stimulants then take only 1/2 tablet after breakfast.

– Since Vitamin B complex (B1, B2, B3, B6, B12, Folate) play very important role in dealing with ADHD I recommand getting B complex with a good quality multivitamin-mineral formula which is high in B vitamins. One of my favourite ones is Healthy Mega (HealthAid) as it is not only high in B vitamins and at the same time it contains zinc, selenium, herbs, digestive enzymes, micronutrients, and few super grasses. Compared with other popular formulas Healthy mega may contain even up to 60 times more vitamins per tablet!
 Adults may take 1 tablet of Healthy Mega after breakfast, children 1/2 tablet (or less) crushed and mixed with juice after breakfast.
Adults may take 1 tablet of Healthy Mega after breakfast, children 1/2 tablet (or less) crushed and mixed with juice after breakfast.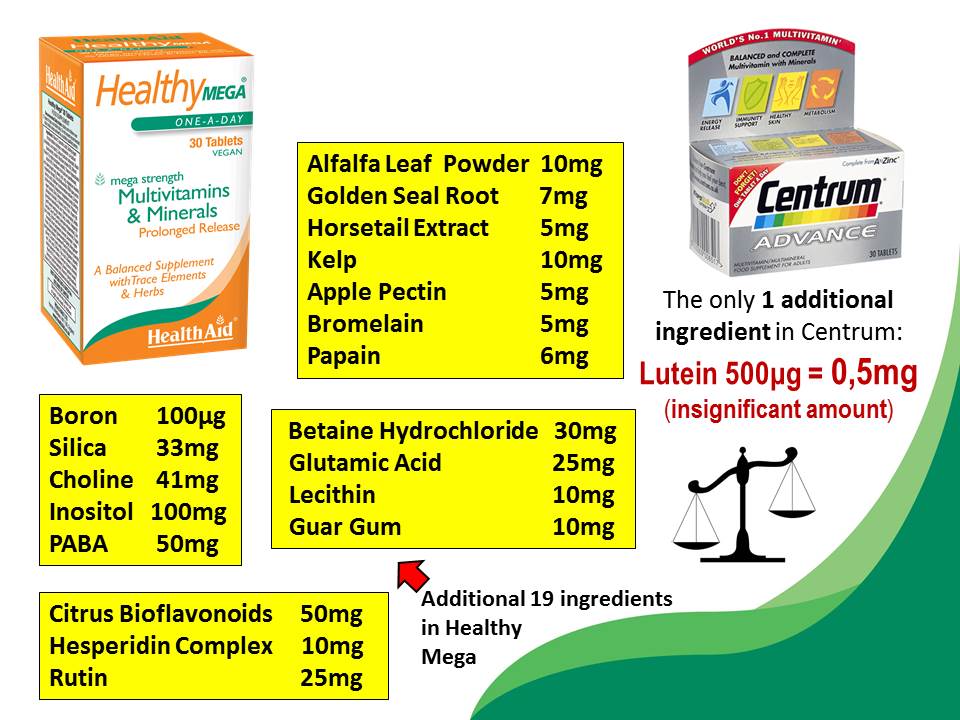
– Beneficial herbs: Tulsi (Holy basil), Lemon balm (Melissa), Turmeric, Valerian root, Chamomile, Hops.
AN ATTEMPT TO SOLVE THE MYSTERY OF AN AUTOIMMUNE RESPONSE
(IT IS VERY IMPORTANT PART! PLEASE READ EVERYTHING!)
Autoimmune diseases are becoming extremely common nowadays, especially among women. Researchers have proved that all autoimmune disorders basically reflect the same strange phenomenon: The irritated and weakened by different factors (including unhealthy diet, dairy, gluten, toxins, stress, or vitamin D deficiency) immune system, mistakes healthy tissue or organs as foreign and begins to attack them. The only difference between numerous autoimmune diseases is the type of organ or tissue which is attacked. In case of vitiligo, eczema or psoriasis it is skin; in Parkinson’s disease it is dopamine producing brain cells; in lupus it can be different parts of the body including joints, skin, liver, etc. When leukocytes attack pancreas they cause type I diabetes. With ulcerative colitis and Crohn’s disease, it is the colon; and with multiple sclerosis, it is the nerve cells of the brain and spinal cord. In case of Hashimoto’s hypothyroidism and Graves’ hyperthyroidism, the thyroid is the target of the immune system.
It is very interesting that Hashimoto’s disease (the most common cause of underactive thyroid) as well as Grave’s disease (the most common cause of overactive thyroid) are both an autoimmune conditions. However, there is an important difference between these two diseases with regards to the role and influence of the immune system: In Hashimoto’s leukocytes, instead of protecting the gland, strangely treat thyroid cells as if they were some dangerous invaders and destroy thyroid cells making them unable to produce enough hormones. In Grave’s disease, on the other hand, white blood cells go into another extreme, and although there is no physiological need to do this, they stimulate thyroid to make way too much of its hormones.
It means that in both cases the immune system gets “crazy” and instead of protecting thyroid cells it behaves in a very strange way and either decides to kill thyroid gland or cause another harm by forcing overproduction of thyroid hormones!
Unfortunately, it is almost impossible to find a medical website or a scientist that would at least attempt to explain this extremely weird behaviour of human immune system. They are unable to do it probably because scientists look for a very complex scientific answers while the solution may be surprisingly simple and logical. Apart from that, for them the immune system is just a bunch of unintelligent cells that came into existence as a result of evolution and only mechanically perform their physiological functions.
Fortunately, back in Poland I was very lucky to have a privilege of translating a series of health lectures by American physician Dr. Sang Lee who developed a very interesting explanation of this phenomenon. So let me try to share with you a few thoughts I still remember from his fascinating and unique health seminars.

When we carefully study the physiology of our immune system we quickly get an impression that somehow our immune system behaves in an incredibly intelligent way. It is also clear that the immune system is very closely connected to the brain and nervous system and that white blood cells respond to different physiological and even psychological needs. One scientist trying to express this idea even suggested that leukocytes behave like “pieces of brain scattered all over the body”.
There is no doubt brain is the most important part of human body. Brain in our organism is like a “king” or a “boss” and because of that, no cell, including the immune system cells ever question any information, signals or anything coming from the brain. That is why the placebo or nocebo effect (a positive or negative attitude of the brain) can impose such a powerful effect on body’s physiology and health.
Knowing this we can draw some very important conclusions which will help us to understand how mental attitudes and emotions can influence the immune system cells to either destroy thyroid or stimulate it to make more hormones.
We know that great majority of both hypothyroidism and hyperthyroidism are caused by abnormal and harmful response (behaviour) of the immune system. The autoimmune form of hypothyroidism is called Hashimoto’s disease and in case of hyperthyroidism it is Graves disease.
Another fact we need to take into consideration is that autoimmune diseases (including both thyroid autoimmune conditions) are much more prevalent among women than man, even if their diet and lifestyle are similar. Now, that doesn’t mean bad diet, and lack of exercise do not contribute to the development of autoimmune diseases, but that there is another cause which should be regarded as even more significant.
The simple conclusion, therefore, is that it is anxiety, depression, worrying and negative mental attitudes that must greatly contribute to the development of autoimmune diseases, simply because poor mental health is also much more common among women than men.
Taking into consideration all those facts Dr Lee suggested that when a woman suffers from chronic anxiety or depression, when she has negative attitude toward life, keeps on thinking about death or suicide, or if she is overwhelmed by any other negative thoughts and emotions, her intelligent and closely connected to the brain immune system gets a clear impression that the “boss” (which is the brain) doesn’t want to live. Therefore, like obedient soldiers the white blood cells feel obliged to fulfil the desire of the “boss”, so they turn against its own body and begin to attack different organs. In case of Hashimoto’s disease it is thyroid.
The whole situation is made even more dangerous when a depressed woman does not exercise, and since only dead body does not move, the leukocytes draw a conclusion that she is already dead so why they should protect the dead body? If she is dead it is more reasonable rather to attack the body and accelerate the decaying process!
But, someone may argue that, if pessimism, depression, anxiety, and suicidal thoughts contribute to the development of autoimmune diseases, how to explain that sometimes babies or small children are diagnosed with autoimmune diseases such as lupus, eczema, or type 1 diabetes? They couldn’t trigger these conditions through their pessimism.
The answer is obvious, they either inherited overreacting immune system or their immune system was negatively influenced by mother’s nervous system (depression, anxiety, suicidal thoughts, etc.) when they were in their mother’s womb. There are many women who during pregnancy were depressed or even attempted to commit suicide and gave birth to children who sooner or later were diagnosed with autoimmune diseases. In addition babies are very often deficient in Vitamin D ad are fed with cow’s milk and it is scientifically proved that both factors also contribute to the development of autoimmune diseases in children.
There are also some nutritional ways to trigger an autoimmune reaction. We already know that heated animal protein, especially the one found in cow’s milk and dairy, is often treated by human immune system as a foreign invader. Because of that leukocytes send antibodies against those heated proteins which get into human body with milk and dairy products. The problem however is that in our bodies there are certain proteins which look exactly like those heated milk proteins so the weakened immune system often mistakenly and simultaneously attack also those body’s own proteins, causing different autoimmune problems.

Apart from pessimism and sedentary lifestyle there are still other “death signals” that may “inspire” the immune system to attack own body. For instance, using stimulants such as alcohol, smoking, illegal drugs, coffee, tea, cola, sugar, etc. could be discerned by the immune system as the “death wish” (“death signals”) of the brain and thus “inspire” the immune system with the idea that the “boss” wishes to die (due to the suicidal lifestyle and diet). The immune system may get this impression because stimulants are harmful and toxic chemicals which slowly contribute to the death of the body.

Also regular consumption of meat products may trigger similar reaction because meat comes from dead animals.
In addition, any heated (cocked, boiled, fried, grilled) animal protein always triggers immune reaction causing leukocytes to start mobilising and thus leading to increased number of leukocytes in the blood. This phenomenon is called leucocytosis and has bad influence on the immune system. As a result of frequent consumption of heated animal proteins (cooked dairy, meat, poultry, fish, or eggs) the immune system is frequently alarmed, has to overwork and may change its nature. Eventually it often turns against its own body causing numerous autoimmune diseases, including thyroid problems.
In case of the Graves hyperthyroidism, however, the behaviour of the immune system seems to be very opposite than in Hashimoto’s thyroiditis or other autoimmune conditions because in Graves hyperthyroidism instead of attacking and destroying the tissue leukocytes just stimulate thyroid to make even more hormones! Now, why on earth in this case the immune system changed its tactics and instead of killing thyroid gland it just decides to “help” it to work very hard?
Well, also in this case Dr Lee got a very interesting explanation. He suggests that if a woman lives a very stressful lifestyle, always tries to do her best in performing her duties at home and work, often in a hurry, dealing with many different things at the same time, if she doesn’t rest and sleep long enough at night, gets often nervous or irritated, drinks coffee or uses other stimulants to increase her energy so that she could be more efficient, then guess what the “intelligent” immune system, which responds to the physiological and psychological needs, do? The immune system says, “Ok, the boss is very restless, wants be more energetic and efficient in performing different duties, let us then go to thyroid and stimulate it to make more hormones, and in this way we will fulfil the wish of the boss.” When over a decade ago I heard this idea for the fists time I said, “Wow! It is so fascinating how our immune system works and how it can be influenced by mental attitudes!”
Well, if this idea is true, and to be honest I personally like it very much, then the best way to prevent and treat autoimmune diseases (including Hashimoto’s hypothyroidism and Graves hyperthyroidism) is by stress control, positive thinking, laughter, frequent smiling, taking care of others, helping people in need, going for a walk and enjoying life and the beauty of the nature. It can be done by avoiding “death signals” (stimulants, meat products and other heated dead foods, etc.). In this way you will show the immune system that you want to live and actually enjoy life. As a result those smart and intelligent invisible tiny soldiers (the white blood cells) will never attack your own body (or will stop doing that) but will protect and fight for you like Kamikazes. Unfortunately, from my long experience I know that for many of us it is very difficult and often even impossible to become a positive thinking person because those negative emotions and fears seem to be part of our nature. Sometimes we even feel like slaves of pessimism. And that is the reason I want to recommand to you a very special, unique and even most important section called “EMPOWERMENT”. So please read it carefully and after that go also to the “GOSPEL OF FREEDOM“, as it reveals the secret of finding the only source of true inward “peace” which according to Apostle Paul “surpasses all knowledge” and which can “guard (protect) our hearts and minds (emotions)”.
Please read this extremely important part (LINK) very carefully as it reveals the secret of finding true source of strength necessary to overcome bad habits and will help you to gain a powerful motivation to not only practice but also enjoy the new and very healthy way of life.
Combined with true strong faith this message will lead you to freedom from negative emotions such as anxiety or existential fears (one of the key source of deadly free radicals). It will empower you with moral strength necessary to overcome long-cultivated bad habits or addictions, often impossible to defeat on our own. This unique and most wonderful good news of the gospel will also give you a powerful motivation to not only practice but also enjoy the new and very healthy way of life.
SOURCES
Hafström I, Ringertz B, Spångberg A, et al. A vegan diet free of gluten improves the signs and symptoms of rheumatoid arthritis: the effects on arthritis correlate with a reduction in antibodies to food antigens. Rheumatology (Oxford) 2001, 40:1175-1179.
Proudman SM, James MJ, Spargo LD, et al. Fish oil in recent onset rheumatoid arthritis: a randomised, double-blind controlled trial within algorithm-based drug use. Ann Rheum Dis 2013.
Tursi A, Brandimarte G, Papa A, et al. Treatment of relapsing mild-to-moderate ulcerative colitis with the probiotic VSL#3 as adjunctive to a standard pharmaceutical treatment: a double-blind, randomized, placebo-controlled study. Am J Gastroenterol 2010, 105:2218-2227.
Share this article!
Chapter 9 from the book “China Study”
by T. Colin Campbell
No GROUP OF DISEASES is more insidious than autoimmune diseases. They are difficult to treat, and progressive loss of physical and mental function is a common outcome. Unlike heart disease, cancer, obesity and Type 2 diabetes, with autoimmune diseases the body systematically attacks itself. The afflicted patient is almost guaranteed to lose.
A quarter million people in the u.s. are diagnosed with one of the forty separate autoimmune diseases each year. I. Women are 2.7 times more likely to be afflicted than are men. About 3% of Americans (one in every thirty-one people) have an autoimmune disease, a staggering total of 8.5 million people; some people put the total at as many as 12-13 million people.3
The more common of these diseases are listed in Chart 9.1. 2 The first nine comprise 97% of all autoimmune disease cases. 2 The most studied are multiple sclerosis (MS), rheumatoid arthritis, lupus, Type 1 diabetes and rheumatic heart disease. 2 These are also the primary autoimmune diseases that have been studied in reference to diet.
Others not listed in Chart 9.1 include inflammatory bowel disease,4 Crohn’s disease,4 rheumatic heart disease3 and (possibly) Parkinson’s disease.s Each disease name may sound very different, but as one recent review points out,2 ” .. . it is important to consider … these disorders as a group.” They show similar clinical backgrounds,3.6. 7 they sometimes occur in the same person and they are often found in the same populations. 2 MS and Type 1 diabetes, for example, have “nearly identical Graves’ disease (Hyperthyroidism) 10. Sjogren’s disease Rheumatoid arthritis 1l. Myasthenia gravis Thyroiditis (Hypothyroidism) 12. Polymyositis/dermatomyositis Vitiligo 13. Addison’s disease Pernicious anemia 14. Scleroderma Glomerulonephritis 15. Primary biliary cirrhosis Multiple sclerosis 16. Uveitis Type 1 diabetes 17. Chronic active hepatitis Systemic lupus erythematosus ethnic and geographic distribution.”8 Autoimmune diseases in general become more common the greater the distance from the equator. This phenomenon has been known since 1922.9 MS, for example, is over a hundred times more prevalent in the far north than at the equator. 10 Because of some of these common features, it is not too far-fetched to think of the autoimmune diseases as one grand disease living in different places in the body and taking on different names. We refer in this way to cancer, which is specifically named depending on what part of the body it resides in.
All autoimmune diseases are the result of one group of mechanisms gone awry, much like cancer. In this case, the mechanism is the immune
system mistakenly attacking cells in its own body. Whether it is the pan-
creas as in Type 1 diabetes, the myelin sheath as in MS or joint tissues
as in arthritis, all autoimmune diseases involve an immune system that
has revolted. It is an internal mutiny of the worst kind, one in which our
body becomes its own worst enemy.
IMMUNITY FROM INVADERS
The immune system is astonishingly complex. I often hear people
speaking about this system as if it were an identifiable organ like a lung.
Nothing could be further from the truth. It is a system, not an organ.
In essence, our immune system is like a military network designed to de-
fend against foreign invaders. The “soldiers” of this network are the white
blood cells, which are comprised of many different sub-groups, each having
its own mission. These sub-groups are analogous to a navy, army, air force
and marines, with each group of specialists doing highly specialized work.
AUTOIMMUNE DISEASES 185
The “recruitment center” for the system is in the marrow of our
bones. The marrow is responsible for generating specialized cells
called stem cells. Some of these cells are released into circulation for
use elsewhere in the body; these are called B-cells (for bone). Other
cells formed in the bone marrow remain immature, or unspecialized,
until they travel to the thymus (an organ in the chest cavity just above
the heart) where they become specialized; these are called T-cells (for
thymus). These “soldier” cells, along with other specialized cells, team
up to create intricate defense plans. They meet at major intersections
around the body, including the spleen (just inside the left lower rib
cage) and the lymph nodes. These meeting points are like command
and control centers, where the “soldier cells” rearrange themselves into
teams to attack foreign invaders.
These cells are remarkably adaptable when they form their teams.
They are able to respond to different circumstances and different for-
eign substances, even those they have never before seen. The immune
response to these strangers is an incredibly creative process. It is one of
the true wonders of nature.
The foreign invaders are protein molecules called antigens. These
foreign cells can be a bacterium or a virus looking to corrupt the body’s
integrity So when our immune system notices these foreign cells, or
antigens, it destroys them. Each of these foreign antigens has a sepa-
rate identity, which is determined by the sequence of amino acids that
comprises its proteins. It is analogous to each and every person having
a different face. Because numerous amino acids are available for creating
proteins, there are infinite varieties of distinctive “faces. “
To counter these antigens, our immune system must customize its
defense to each attack. It does this by creating a “mirror image” pro-
tein for each attacker. The mirror image is able to fit perfectly onto the
antigen and destroy it. Essentially, the immune system creates a mold
for each face it encounters. Every time it sees that face after the initial
encounter, it uses the custom-made mold to “capture” the invader and
destroy it. The mold may be a B-cell antibody or a T-cell-based receptor
protein.
Remembering each defense against each invader is what immuniza-
tion is all about. An initial exposure to chicken pox, for example, is a
difficult battle, but the second time you encounter that virus you will
know exactly how to deal with it, and the war will be shorter, less pain-
ful and much more successful. You may not even get sick. 186 THE CHINA STUDY
IMMUNITY FROM OURSELVES
Even though this system is a wonder of nature when it is defending the
body against foreign proteins, it is also capable of attacking the same
tissues that it is designed to protect. This self-destructive process is
common to all autoimmune diseases. It is as if the body were to commit
suicide.
One of the fundamental mechanisms for this self-destructive behav-
ior is called molecular mimicry. It so happens that some of the foreign
invaders that our soldier cells seek out to destroy look the same as our
own cells. The immune system “molds” that fit these invaders also fit
our own cells. The immune system then destroys, under some circum-
stances, everything that fits the mold, including our own cells. This is
an extremely complex self-destructive process involving many different
strategies on the part of the immune system, all of which share the same
fatal flaw of not being able to distinguish “foreign” invader proteins
from the proteins of our own body.
What does all of this have to do with what we eat? It so happens that
the antigens that trick our bodies into attacking our own cells may be
in food. During the process of digestion, for example, some proteins
slip into our bloodstream from the intestine without being fully broken
down into their amino acid parts. The remnants of undigested proteins
are treated as foreign invaders by our immune system, which sets about
making molds to destroy them and sets into motion the self-destructive
autoimmune process.
One of the foods that supply many of the foreign proteins that mimic
our own body proteins is cow’s milk. Most of the time, our immune
system is quite smart. Just like an army arranges for safeguards against
friendly fire, the immune system has safeguards to stop itself from at-
tacking the body it’s supposed to protect. Even though an invading
antigen looks just like one of the cells in our own body, the system can
still distinguish our own cells from the invading antigen. In fact, the im-
mune system may use our own cells to practice making molds against
the invader antigen without actually destroying the friendly cell.
This is analogous to training camps in preparations for war. When our
immune system is working properly, we can use the cells in our body that
look like the antigens as a training exercise, without destroying them, to
prepare our soldier cells to repulse the invading antigens. It is one more
example l of the exceptional elegance of nature’s ability to regulate itself. AUTOIMMUNE DISEASES 187
The immune system uses a very delicate process to decide which pro-
teins should be attacked and which should be left alone. ll The way this
process, which is incredibly complex, breaks down with autoimmune
diseases is not yet understood. We just know that the immune system
loses its ability to differentiate between the body’s cells and the invading
antigen, and instead of using the body’s cells for “training,” it destroys
them along with the invaders.
TYPE 1 DIABETES
In the case of Type 1 diabetes, the immune system attacks the pancreas
cells responsible for producing insulin. This devastating, incurable
disease strikes children, creating a painful and difficult experience for
young families. What most people don’t know, though, is that there is
strong evidence that this disease is linked to diet and, more specifically,
to dairy products. The ability of cow’s milk protein to initiate Type 1
diabetes 12
–
14 is well documented. The possible initiation of this disease
goes like this:
• A baby is not nursed long enough and is fed cow’s milk protein,
perhaps in an infant formula.
• The milk reaches the small intestine, where it is digested down to
its amino acid parts.
• For some infants, cow’s milk is not fully digested, and small amino
acid chains or fragments of the original protein remain in the in-
testine.
• These incompletely digested protein fragments may be absorbed
into the blood.
• The immune system recognizes these fragments as foreign invad-
ers and goes about destroying them.
• Unfortunately, some of the fragments look exactly the same as the
cells of the pancreas that are responsible for making insulin.
• The immune system loses its ability to distinguish between the
cow’s milk protein fragments and the pancreatic cells, and destroys
them both, thereby eliminating the child’s ability to produce insu-
lin.
• The infant becomes a Type 1 diabetic, and remains so for the rest
of his or her life.
This process boils down to a truly remarkable statement: cow~ milk
may cause one of the most devastating diseases that can befall a child. For
obvious reasons, this is one of the most contentious issues in nutrition
today.
One of the more remarkable reports on this cow’s milk effect was
published over a decade ago, in 1992, in the New England Journal of
Medicine. 12 The researchers, from Finland, obtained blood from Type
1 diabetic children, aged four to twelve years. Then they measured the
levels of antibodies that had formed in the blood against an incomplete-
ly digested protein of cow’s milk called bovine serum albumin (BSA).
They did the same process with non-diabetic children and compared
the two groups (remember, an antibody is the mirror image, or “mold,”
of a foreign antigen) . Children who had antibodies to cow’s milk protein
must have previously consumed cow’s milk. It also means that undi-
gested protein fragments of the cow’s milk proteins had to have entered
the infant’s circulation in order to cause the formation of antibodies in
the first place.
The researchers discovered something truly remarkable. Of the 142
diabetic children measured, every Single one had antibody levels higher
than 3.55. Of the seventy-nine normal children measured, every single
one had antibody levels less than 3.55.
There is absolutely no overlap between antibodies of healthy and
diabetic children. All of the diabetic children had levels of cow’s milk
antibodies that were higher than those of all of the non-diabetic chil-
dren. This implies two things: children with more antibodies consumed
more cow’s milk, and second, increased antibodies may cause Type 1
diabetes.
These results sent shock waves through the research community. It
was the complete separation of antibody responses that made this study
so remarkable. This study,12 and others even earlier,15-17 initiated an ava-
lanche of additional studies over the next several years that continue to
this day. 13. 18. 19
Several studies have since investigated this effect of cow’s milk on
BSA antibody levels. All but one showed that cow’s milk increases BSA
antibodies in Type 1 diabetic children,18 although the responses were
quite variable in their magnitude.
Over the past decade, scientists have investigated far more than
just the BSA antibodies, and a more complete picture is coming into
view. Very briefly, it goes something like this 13
, 19: infants or very young
children of a certain genetic background,2o,21 who are weaned from the
breast too early22 onto cow’s milk and who, perhaps, become infected AUTOIMMUNE OISEASES 189
with a virus that may corrupt the gut immune system,l9 are likely to
have a high risk for Type 1 diabetes. A study in Chile 23 considered the
first two factors, cow’s milk and genes. Genetically susceptible children
weaned too early onto cow’s milk-based formula had a risk of Type 1 di-
abetes that was 13.1 times greater than children who did not have these
genes and who were breast-fed for at least three months (thus minimiz-
ing their exposure to cow’s milk). Another study in the U.S. showed that
genetically susceptible children fed cow’s milk as infants had a risk of
disease that was 11.3 times greater than children who did not have these
genes and who were breast-fed for at least three months. 24 This eleven
to thirteen times greater risk is incredibly large (1,000-1,200%!); any-
thing over three to four times is usually considered very important. To
put this in perspective, smokers have approximately ten times greater
risk of getting lung cancer (still less than the eleven to thirteen times
risk here) and people with high blood pressure and cholesterol have a
2.5-3.0 times greater risk of heart disease (Chart 9.2) .18
So how much of the eleven to thirteen times increased risk of Type
1 diabetes is due to early exposure to cow’s milk, and how much is due
to genes? These days, there is a popular opinion that Type 1 diabetes is
due to genetics, an opinion often shared by doctors as well. But genetics
alone cannot account for more than a very small fraction of cases of this
disease. Genes do not act in isolation; they need a trigger for their ef-
fects to be produced. It has also been observed that after one member of
identical twin pairs gets Type 1 diabetes, there is only a 13-33% chance
of the second twin getting the disease, even though both twins have
the same genes. l3
, 20, 21, 25. 26
If it were all due to genes, closer to lOO% of
the identical twins would get the disease. In addition, it is possible that
the 13-33% risk for the second twin is due to the sharing of a common
environment and diet, factors affecting both twins.
Consider, for example, the observation shown in Chart 9.3, which
highlights the link between one aspect of environment, cow’s milk con-
sumption, and this disease. Cow’s milk consumption by children zero
to fourteen years of age in twelve countries 27 shows an almost perfect
correlation with Type 1 diabetes. 28 The greater the consumption of
cow’s milk, the greater the prevalence of Type 1 diabetes. In Finland,
Type 1 diabetes is thirty-six times more common than in Japan. 29 Large
amounts of cow’s milk products are consumed in Finland but very little
is consumed in JapanY
Cow Milk Consumption (liters/person/year) AUTOIMMUNE DISEASES 191
As we have seen with other diseases of affluence, when people migrate
from areas of the world where disease incidence is low to areas of the
world where disease incidence is high, they quickly adopt the high inci-
dence rates as they change their diet and lifestyle.
This shows that even
though individuals may have the necessary gene(s), the disease will occur
only in response to certain dietary and/or environmental circumstances.
Disease trends over time show the same thing. The worldwide preva-
lence of Type 1 diabetes is increasing at an alarming rate of 3% per year.
33
This increase is occurring for different populations even though there
may be substantial differences in disease rates. This relatively rapid in-
crease cannot be due to genetic susceptibility. The frequency of anyone
gene in a large population is relatively stable over time, unless there are
changing environmental pressures that allow one group to reproduce
more successfully than another group. For example, if all families with
Type 1 diabetic relatives had a dozen babies and all the families without
Type 1 diabetic relatives died off, then the gene or genes that may be
responsible for Type 1 diabetes would become much more common in
the population. This, of course, is not what is happening, and the fact
that Type 1 diabetes is increasing 3% every year is very strong evidence
that genes are not solely responsible for this disease.
It seems to me that we now have impressive evidence shOWing that
cow’s milk is likely to be an important cause of Type 1 diabetes. When
the results of all these studies are combined (both genetically suscep-
tible and not susceptible), we find that children weaned too early and
fed cow’s milk have, on average, a 50-60% higher risk of Type 1 diabetes
(1.5-1.6 times increased risk).34
The earlier information on diet and Type 1 diabetes was impressive
enough to cause two Significant developments. The AmericanAcademy
of Pediatrics in 1994 “strongly encouraged” that infants in families
where diabetes is more common not be fed cow’s milk supplements for
their first two years of life. Second, many researchers
19
have developed
prospective studies-the kind that follow individuals into the future-
to see if a careful monitoring of diet and lifestyle could explain the onset
of Type 1 diabetes.
Two of the better known of these studies have been underway in Fin-
land, one starting in the late 1980S
15
and the other in the mid-1990s.
35
One has shown that cow’s milk consumption increases the risk of Type
1 diabetes five- to sixfold,36 while the second
35
tells us that cow’s milk
increases the development of at least another three to four antibodies 192 THE CHINA STUDY
in addition to those presented previously (p. 190). In a separate study,
antibodies to beta-casein, another cow’s milk protein, were significantly
elevated in bottle-fed infants compared to breast-fed infants; children
with Type 1 diabetes also had higher levels of these antibodies.
37
In
short, of the studies that have reported results, the findings strongly
confirm the danger of cows milk, especially for genetically susceptible
children.
THE CONTROVERSY OF CONTROVERSY
Imagine looking at the front page of the newspaper and finding the
following headline: “Cow’s Milk the Likely Cause of Lethal Type 1
Diabetes.” Because the reaction would be so strong, and the economic
impact monumental, this headline won’t be written anytime soon,
regardless of the scientific evidence. Stifling this headline is accom-
plished under the powerful label of “controversy.” With so much at
stake, and so much information understood by so few people, it is easy
to generate and sustain controversy. Controversies are a natural part
of science. Too often, however, controversy is not the result of legiti-
mate scientific debate, but instead reflects the perceived need to delay
and distort research results. For example, if I say cigarettes are bad for
you and provide a mountain of evidence to support my contention,
the tobacco companies might come along and pick out one unsolved
detail and then claim that the whole idea of cigarettes being unhealthy
is mired in controversy, thereby nullifying all my conclusions. This is
easy to do, because there will always be unsolved details; this is the
nature of science. Some groups use controversy to stifle certain ideas,
impede constructive research, confuse the public and turn public
policy into babble rather than substance. Sustaining controversy as a
means of discrediting findings that cause economic or social discom-
fort is one of the greatest sins in science.
It can be difficult for the layperson to assess the legitimacy of a highly
technical controversy such as that regarding cow’s milk and Type 1 dia-
betes. This is true even if the layperson is interested in reading scientific
articles.
Take a recent scientific review
38
of the cow’s milk-Type 1 diabetes
association. In ten human studies (all case-control) summarized in a
paper published as part of a “controversial topics series,”38 the authors
concluded that five of the ten studies showed a statistically Significant
positive association between cow’s milk and Type 1 diabetes and five did L
not. Obviously, this at first seems to demonstrate considerable uncer-
tainty, going a long way to discredit the hypothesis.
However, the five studies that were counted as “negative” did not
show that cow’s milk decreased Type 1 diabetes. These five studies
showed no statistically significant effect either way. In contrast, there
are a total of five statistically significant studies and all five showed the
same result: early cow’s milk consumption is associated with increased
risk of Type 1 diabetes. There is only one chance in sixty-four that this
was a random or chance result.
There are many, many reasons, some seen and some unseen, why an
experiment would find no statistically significant relationship between
two factors, even when a relationship really exists. Perhaps the study
didn’t include enough people, and statistical certainty was unattainable.
Perhaps most of the subjects had very similar feeding practices, limiting
detection of the relationship you might otherwise see. Maybe trying to
measure infant feeding practices from years ago was inaccurate enough
that it obscured the relationship that does exist. Perhaps the researchers
were studying the wrong period of time in an infant’s life.
The point is, if five of the ten studies did find a statistically significant
relationship, and all five showed that cow’s milk consumption is linked
to increasing Type 1 diabetes, and none show that cow’s milk consump-
tion is linked to decreasing Type 1 diabetes, I could hardly justify say-
ing, as the authors of this review did, that the hypothesis “has become
quite murky with inconsistencies in the literature. “38
In this same review,38 the authors summarized additional studies that
indirectly compared breast-feeding practices associated with cow’s milk
consumption and Type 1 diabetes. This compilation involved fifty-two
possible comparisons, twenty of which were statistically significant. Of
these twenty significant findings, nineteen favored an association of cows
milk with disease, and only one did not. Again the odds heavily favored the
hypotheSized association, something that the authors failed to note.
I cite this example not only to support the evidence showing a cow’s
milk effect on Type 1 diabetes, but also to illustrate one tactic that is
often used to make something controversial when it is not. This practice
is more common than it should be and is a source of unnecessary con-
fusion. When researchers do this-even if they do it unintentionally-
they often have a serious prejudice against the hypothesis in the first
place. Indeed, shortly after I wrote this, I heard a brief National Public
Radio interview on the Type 1 diabetes problem with the senior author of this review paper.38 Suffice it to say, the author did not acknowledge
the evidence for the cow’s milk hypothesis.
Because this issue has mammoth financial implications for American
agriculture, and because so many people have such intense personal
biases against it, it is unlikely that this diabetes research will reach the
American media anytime soon. However, the depth and breadth of evi-
dence now implicating cow’s milk as a cause of Type 1 diabetes is over-
whelming, even though the very complex mechanistic details are not
yet fully understood. We not only have evidence of the danger of cow’s
milk, we also have considerable evidence showing that the association
between diabetes and cow’s milk is biologically plausible. Human breast
milk is the perfect food for an infant, and one of the most damaging
things a mother can do is to substitute the milk of a cow for her own.
Multiple sclerosis (MS) is a particularly difficult autoimmune disease, both for those who have it and for those who care for its victims. It is a lifelong battle involving a variety of unpredictable and serious disabilities. MS patients often pass through episodes of acute attacks while gradually losing their ability to walk or to see. After ten to fifteen years, they often are confined to a wheelchair, and then to a bed for the rest of their lives. About 400,000 people in the U.S. alone have the disease, according to the National Multiple Sclerosis Society.39 It is a disease that is initially diagnosed between twenty and forty years of age and strikes women about three times more often than men. Even though there is widespread medical and scientific interest in this disease, most authorities claim to know very little about causes or cures. Major multiple sclerosis Internet Web sites all claim that the disease is an enigma. They generally list genetics, viruses and environ-mental factors as possibly playing roles in the development of this dis-ease but pay almost no heed to a possible role for diet. This is peculiar considering the wealth of intriguing information on the effects of food that is available from reputable research reports. Once again cow’s milk appears to play an important role. The “multiple” symptoms of this disease represent a nervous system gone awry. The electrical signals carrying messages to and from the central nervous system (brain and spinal cord) and out through the peripheral nervous system to the rest of the body are not well coordinated l and controlled. This is because the insulating cover or sheath of the nerve fibers, the myelin, is being destroyed by an autoimmune reaction. Think of what would happen to your household wiring if the electrical insulation became thin or was stripped away, leaving bare wires. The electrical Signals would be short-circuited. That is what happens with MS; the wayward electrical signals may destroy cells and “burn” patches of neighboring tissue, leaVing little scars or bits of sclerotic tissue. These “burns” can become serious and ultimately destroy the body. The initial research showing an effect of diet on MS goes back more than half a century to the research of Dr.
Roy Swank, who began his work in Norway and at the Montreal Neurological Institute during the 1940s. Later, Dr. Swank headed the Division of Neurology at the University of Oregon Medical Schoo1.43 Dr. Swank became interested in the dietary connection when he learned that MS appeared to be more common in the northern climates. There is a huge difference in MS prevalence as one moves away from the equator: MS is over 100 times more prevalent in the far north than at the equator,l° and seven times more prevalent in south Australia (closer to the South Pole) than in north Australia.44 This distribution is very similar to the distribution of other autoimmune diseases, including Type 1 diabetes and rheumatoid arthritis. 45,46 Although some scientists speculated that magnetic fields might be responsible for the disease, Dr. Swank thought it was diet, especially animal-based foods high in saturated fats.43 He found that inland dairy-consuming areas of Norway had higher rates of MS than coastal fish-consuming areas.
Dr. Swank conducted his best-known trial on 144 MS patients recruited from the Montreal Neurological Institute. He kept records on these patients for the next thirty-four years Y He advised his patients to consume a diet low in saturated fat, most of whom did, but many of whom did not. He then classified them as good dieters or poor dieters, based on whether they consumed less than 20 gl day or more than 20 gl day of saturated fat. (For comparison, a bacon cheeseburger with condiments has about sixteen grams of saturated fat. One small frozen chicken pot pie has almost ten grams of saturated fat.) As the study continued, Dr. Swank found that progression of disease was greatly reduced by the low-saturated fat diet, which worked even for people with initially advanced conditions. He summarized his work in 1990, concluding that for the sub-group of patients who began the low-saturated fat diet during the earlier stages of their disease, “about 95% .. . remained only mildly disabled for approximately thirty years. “Only 5% of these patients died. In contrast, 80% of the patients with early-stage MS who consumed the “poor” diet (higher saturated fat) died of MS. The results from all 144 patients, including those who started the diet at a later stage of disease, are shown in Chart 9.4. This work is remarkable. To follow people for thirty-four years is an exceptional demonstration of perseverance and dedication. Moreover, if this were a study testing a potential drug, these findings would make any pharmaceutical manufacturer jingle the coins in his or her pocket. Swank’s first results were published more than a half century ago, then again and again and again47 for the next forty years. More recently, additional studies have confirmed and extended Swank’s observations and gradually have begun to place more emphasis on cow’s milk. These new studies show that consuming cow’s milk is strongly linked to MS both when comparing different countries52 and when comparing states within the U.S.51 Chart 9.5, published by French researchers, compares the consumption of cow’s milk with MS for twenty-six populations in twenty-four countries. 52 This relationship, which is virtually identical to that for Type 1 diabetes, is remarkable, and it is not due to variables such as the avail-ability of medical services or geographic latitude. 51 In some studies researchers suggest this strong correlation with fresh cow’s milk might ci.. be due to the presence of a virus in the milk. These more recent studies also suggest that saturated fat alone probably was not fully responsible for Swank’s results. The consumption of meat high in saturated fat, like milk, was also associated with MS in these multi-country studies,54 while the consumption of fish, containing more omega-3 fat, was associated with low rates of disease. S5 The association of cow’s milk with MS, shown in Chart 9.5, may be impressive, but it does not constitute proof. For example, where do genes and viruses come into play? Each of these, in theory, might ac-count for the unusual geographic distribution of this disease. In the case of viruses, no definite conclusions are yet possible. A variety of different virus types have been suggested and a variety of effects on the immune system may be involved. However, nothing very convincing has been proven. Some of the evidence is based on finding more viral antibodies in MS patients than in controls, some is based on sporadic outbreaks of MS among isolated communities, and some is based on finding virus-like genes among MS cases. With regard to genes, we can begin to puzzle out their association with MS by asking the usual question: what happens to people who migrate from one population to another, keeping their genes the same but changing their diets and their environment? The answer is the same as it was for cancer, heart disease and Type 2 diabetes. People acquire the risk of the population to which they move, especially if they move before their adolescent years. This tells us that this disease is more strongly related to environmental factors than it is to genes. 59 Specific genes have been identified as possible candidates for causing MS but, according to a recent report,3 there may be as many as twenty five genes playing such a role. Therefore, it will undoubtedly be a long time before we determine with any precision which genes or combinations of genes predispose someone to MS. Genetic predisposition may make a difference as to who gets MS, but even at best, genes can only account for about one-fourth of the total disease risk. 60 Although MS and Type 1 diabetes share some of the same unanswered questions on the exact roles of viruses and genes and the immune system, they also share the same alarming evidence regarding diet. For both diseases, a “Western” diet is strongly associated with disease incidence. Despite the efforts of those who would rather dismiss or mire these observational studies in controversy, they paint a consistent picture. Intervention studies conducted on people already suffering from these diseases only reinforce the findings of the observational studies. Dr. Swank did brilliant work on MS, and you may recall from chapter seven that Dr. James Anderson successfully reduced the medication requirements for Type 1 diabetics using diet alone. It’s important to note that both of these doctors used a diet that was significantly more moderate than a total whole foods, plant-based diet. I wonder what would happen to these autoimmune patients if the ideal diet were followed. I would bet on even greater success.
THE COMMONALITY OF AUTOIMMUNE DISEASES
What about other autoimmune diseases? There are dozens of autoim-
mune diseases and I have mentioned only two of the more prominent
ones. Can we say anything about autoimmune diseases as a whole?
To answer this question, we need to identify how much these dis-
eases have in common. The more they have in common, the greater the
probability that they also will share a common cause (or causes). This
is like seeing two people you don’t know, both of whom have a similar
body type, hair color, eye color, facial features, physical and vocal man-
nerisms and age, and concluding that they come from the same parents.
Just as we hypothesized that diseases of affluence such as cancer and AUTOIMMUNE DISEASES 199
heart disease have common causes because they share similar geogra-
phy and similar biochemical biomarkers (chapter four), we can also
hypothesize that MS, Type 1 diabetes, rheumatoid arthritis, lupus and
other autoimmune diseases may share a similar cause if they exhibit
similar characteristics.
First, by definition, each of these diseases involves an immune sys-
tem that has gone awry in such a way that it attacks “self’ proteins that
look the same as foreign proteins.
Second, all the autoimmune diseases that have been studied have
been found to be more common at the higher geographic latitudes
where there is less constant sunshine. 9
• 10, 61
Third, some of these diseases have a tendency to afflict the same
people. MS and Type 1 diabetes, for example, have been shown to coex-
ist in the same individuals. 62
–
65 Parkinson’s disease, a non-autoimmune
disease with autoimmune characteristics, is often found with MS, both
within the same geographic regions 66 and within the same individuals. 5
MS also has been associated-either geographically or within the same
individuals-with other autoimmune diseases like lupus, myasthenia
gravis, Graves’ disease and eosinophilic vasculitis. 63 Juvenile rheuma-
toid arthritis, another autoimmune disease, has been shown to have an
unusually strong association with Hashimoto thyroiditis. 67
Fourth, of those diseases studied in relation to nutrition, the con-
sumption of animal-based foods-especially cow’s milk-is associated
with greater disease risk.
Fifth, there is evidence that a virus (or viruses) may trigger the onset
of several of these diseases.
A sixth and most important characteristic binding together these
diseases is the evidence that their “mechanisms of action” have much
in common-jargon used to describe the “how to” of disease forma-
tion. As we consider common mechanisms of action, we might start
with sunlight exposure, because this somehow seems linked to the au-
toimmune diseases. Sunlight exposure, which decreases with increas-
ing latitude, could be important-but clearly there are other factors .
The consumption of animal-based foods, especially cow’s milk, also
increases with distance from the equator. In fact, in one of the more ex-
tensive studies, cow’s milk was found to be as good of a predictor of MS
as latitude (Le., sunshine)Y In Dr. Swank’s studies in Norway, MS was
less common near the coastal areas of the country where fish intake was
more common. This gave rise to the idea that the omega-3 fats common 200 THE CHINA STUDY
to fish might have a protective effect. What is almost never mentioned,
however, is that dairy consumption (and saturated fat) was much lower
in the fish-eating areas. Is it possible that cow’s milk and lack of sun-
shine are having a similar effect on MS and other autoimmune diseases
because they operate through a similar mechanism? This could be very
interesting, if true.
As it turns out, the idea is not so crazy. This mechanism involves,
once again, vitamin D. There are experimental animal models of lupus,
MS, rheumatoid arthritis and inflammatory bowel disease (e.g., Crohn’s
disease, ulcerative colitis), each of which is an autoimmune disease. 6
• 7. 68
Vitamin D, operating through a similar mechanism in each case, prevents
the experimental development of each of these diseases. This becomes
an even more intriguing story when we think about the effect of food on
vitamin D.
The first step in the vitamin D process occurs when you go outside
on a sunny day. When the sunshine hits your exposed skin, the skin
produces vitamin D. The vitamin D then must be activated in the kid-
ney in order to produce a form that helps repress the development of
autoimmune diseases. As we’ve seen before, this critically important
activation step can be inhibited by foods that are high in calcium and
by acid-producing animal proteins like cow’s milk (some grains also
produce excess acid). Under experimental conditions, the activated
vitamin D operates in two ways: it inhibits the development of certain
T-cells and their production of active agents (called cytokines) that
initiate the autoimmune response, and/or it encourages the production
of other T-cells that oppose this effect. 69. 70 (An abbreviated schematic
of this vitamin D network is shown in Appendix C.) This mechanism
of action appears to be a strong commonality between all autoimmune
diseases so far studied.
Knowing the strength of the evidence against animal foods, cow’s milk
in particular, for both MS and Type 1 diabetes, and knowing how much
in common all of the autoimmune diseases have, it is reasonable to be-
gin thinking about food and its relationship to a much broader group of
autoimmune diseases. ObViously caution is called for; more research is
needed to make conclusive statements about cross-autoimmune disease
similarities. But the evidence we have now is already striking.
Today almost no indication of the dietary connection to these dis-
eases has reached public awareness. The Web site of the Multiple Scle-
rosis International Federation, for example, reads, “There is no credible AUTOIMMUNE DISEASES 201
evidence that MS is due to poor diet or dietary deficiencies.” They warn
that dietary regimens can be “expensive” and “can alter the normal
nutritional balance.”7l If changing your diet is expensive, I don’t know
what they would say about being bedridden and incapacitated. As far as
altering the “normal nutritional balance” is concerned, what is normal?
Does this mean the diet that we now eat is “normal”-the diet that is
largely responsible for diseases that cripple, kill and make profoundly
miserable millions of Americans every year? Are massive rates of heart
disease, cancer, autoimmune diseases, obesity and diabetes “normal”? If
this is normal, I propose we start seriously considering the abnormal.
There are 400,000 Americans who are victims of multiple sclerosis,
and millions more with other autoimmune diseases. While statistics,
research results and clinical descriptions form the basis for much of my
discussion of diet and disease, the importance of the information comes
down to the intimate experience of individual people. Anyone of these
serious diseases I’ve talked about in this chapter can forever alter the
life of any person-a family member, a friend, a neighbor, a coworker
or you yourself.
It is time to sacrifice our sacred cows. Reason must prevail. Profes-
sional societies, doctors and government agencies need to stand up and
do their duty, so that children being born today do not face tragedies
that otherwise could be prevented.


